|
Hypotension
is the medical term for low blood pressure, which
can mean inadequate blood flow to the heart, brain and other vital organs. Blood pressure
is measured in millimeters of mercury (mm HG). For a healthy young adult,
normal
blood pressure is considered to be less than 140mm Hg over 90mm Hg. The first
number - in this case, 140 - is systolic blood pressure, the pressure in the
blood vessels when the heart contracts; the second number - in this case, 90 -
is the pressure between contractions. blood flow to the heart, brain and other vital organs. Blood pressure
is measured in millimeters of mercury (mm HG). For a healthy young adult,
normal
blood pressure is considered to be less than 140mm Hg over 90mm Hg. The first
number - in this case, 140 - is systolic blood pressure, the pressure in the
blood vessels when the heart contracts; the second number - in this case, 90 -
is the pressure between contractions.
The pressure with which the blood is pumped around the circulation varies
between individuals and throughout the day. Blood pressure at the lower end of the
normal range, is not likely to produce symptoms. However if the pressure in the
circulation is below the level needed (90/60 mm Hg to
130/80 mm Hg) to provide the brain with enough blood light
headaches or fainting may occur.
A common type of hypotension is, postural hypotension in which suddenly
standing, or sitting up leads to light headaches and fainting. Postural
hypotension is considered a failure of the autonomic nervous system - the part
of the nervous system that controls involuntary vital actions, such as the
heartbeat - to react appropriately to sudden changes. When you stand up, some
blood pools in your lower extremities. Uncorrected, this would cause your blood
pressure to fall.
|
|
What are the Causes? |
|
|
. |
|
. |
. |
The causes of orthostatic hypotension can be divided into neurogenic and non-neurogenic
categories.
Neurogenic causes:
|
Nonneurogenic Causes of Orthostatic Hypotension |
|
 Cardiac pump failure Cardiac pump failure
Reduced intravascular volume
|
 Venous pooling Venous pooling
-
Alcohol
-
Postprandial dilation of splanchnic vessel beds
-
Vigorous exercise with dilation of skeletal vessel beds
-
Heat: hot environment, hot showers and baths, fever
-
Prolonged recumbency or standing
-
Spesis
Medications
-
Antyhypertensives
-
Diuretics
-
Vasodilators: nitrates, hydralazine (Apresoline)
-
Alpha- and beta-blocking agents
-
Central nervous system sedatives: barbiturates, opiates
-
Tricyclic antidepressants
-
Phenothiazines
|
|
Non-neurogenic causes:
In many people low blood pressure
occurs as a result of dehydration, following loss of large amounts of
fluid or salts from the body. For example heavy sweating, loss of blood or
profuse diarrhea may all causes hypotension.
Disorders that reduce the efficiency of the heart's pumping action are common
cause of blood pressure. These disorders include heart failure, heart
attack and an irregular heart beat.
Hypotension may also be caused by an abnormal widening of the blood vessels
which may occur as a result of an infection in the bloodstream or a serve
allergic reaction.
Postural hypotension may be caused by disorders in which, the nerve supply to
the blood vessels is damaged such as diabetic neuropathy or peripheral
neuropathies. Hypotension may also sometimes be the result of an adverse
effect of certain drugs particularly those used in the treatment of high blood
pressure and certain types of antidepressant
drugs.
|
Neurogenic Causes of Orthostatic Hypotension
|
|
Primary automatic system failure
Secondary autonomic system failure
|
|
Adapted from Engstrom JW, Martin JP. Disorders of
the autonomic nervous system. In: Fauci AS, ed. Harrison's Principles of
internal medicine. New York: McGraw-Hill. In Press. Used with permission. |
You may not have symptoms of hypotension unless your blood pressure is very
low. Symptoms may include.

Postural hypotension, particularly in the elderly, may increase the risk of
falls, leading to the potential for bone fractures and other injuries.
These symptoms, are usually temporary and blood pressure rises when the cause
is treated. However if blood pressure is too low to provide an adequate blood
supply to vital it can be fatal.
Symptoms of dizziness and lightheadedness upon standing do not necessarily
mean that you have postural hypotension. A wide range of underlying conditions,
may cause these symptoms. An accurate diagnosis must be based on repeated
evaluation of blood pressure and pulse rate after you have been lying down for
at least five minutes and then after you stand quietly for one minute and then
for three minutes. A hypotensive response may be immediate or delayed. Prolonged
standing or a tilt test may be needed to detect a delayed hypotensive response.
Test used are listed below: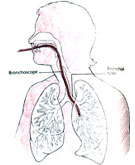
-
Bronchoscopy - a diagnostic procedure in
which a tube with a tiny camera on the end is inserted through the nose or
mouth into the lungs. The procedure provides a view of the airways of the lung
and allows doctors to collect lung secretions and to
biopsy
for tissue specimens.
-
Lung scan- A type of nuclear scan involving
radioactive gallium which helps determine whether a patient has inflammation
in the lungs.
-
 Pulmonary function tests - a broad range of tests that are usually
done in a health care provider's office or a specialized facility. They
measure how well the lungs take in and exhale air and how efficiently they
transfer oxygen into the blood. Spirometry measures how well the lungs exhale.
The information gathered during this test is useful in diagnosing certain
types of lung disorders, but is most useful when assessing for obstructive
lung diseases (especially asthma and chronic obstructive pulmonary disease, COPD). Pulmonary function tests - a broad range of tests that are usually
done in a health care provider's office or a specialized facility. They
measure how well the lungs take in and exhale air and how efficiently they
transfer oxygen into the blood. Spirometry measures how well the lungs exhale.
The information gathered during this test is useful in diagnosing certain
types of lung disorders, but is most useful when assessing for obstructive
lung diseases (especially asthma and chronic obstructive pulmonary disease, COPD).
-
Sputum analysis (if the cough produces sputum) - Sputum is a
secretion that is produced in the lungs and the
bronchi. This mucus-like secretion may become infected, bloodstained,
or contain abnormal cells that may lead to a diagnosis. Sputum is what comes
up with deep coughing. The patient is asked to cough deeply and spit any
sputum in a sterile cup. The sputum is then taken to the laboratory. There, it
is placed in a medium under conditions that allow the organisms to grow.
-
X-ray of the chest- lungs, heart, large arteries, ribs, and
the diaphragm
|
|
Patient's blood pressure will be measured while lying down, and then
standing to find the obvious
reasons for low blood pressure. For example, dehydration might need
treatment with intravenous fluids, those with disorders, such as a heart condition, may be admitted to hospital for tests and treatment. If you medications is
causing hypotension your doctor will probably advise a change of drug or dosage.
|
Treatment of Orthostatic Hypotension
|
|
Nonpharmacologic treatments
-
Avoidance of prolonged standing
-
Slow, careful changes in position,
especially on arising in the morning
-
Avoidance of alcohol
-
Avoidance of hot environments and hot
showers or baths
-
Multiple small meals
-
Avoidance of rigorous exercise
-
Sleeping with lead-up tilt
-
Scheduling of activities in the afternoon
-
Increased salt and fluid intake
Pharmacologic treatments
-
Removal of medications that exacerbate
hypotension, when possible
-
Fludrocortisone (Florinef)
-
Sympathetic antagonists such as midodrine
(ProAmatine) and over-the-counter sympathomimetics
-
Erythropoietin
|
-
Quit smoking or don't smoke in the first place.
-
Stay away from secondhand cigarette smoke and airborne irritants.
-
If you have seasonal allergies like hay fever, stay indoors during days or
seasons when airborne allergens are high and, if possible, keep the windows
closed. Use an air conditioner; avoid using fans that draw in air from
outdoors; avoid air drying your clothes; shower and change your clothes after
being outside.
-
If you have allergies year round, cover your pillows and mattress with
dust mite covers, use an air purifier, avoid pets and other triggers.
-
Get regular exercise to promote blood flow.
-
Avoid
heavy lifting.
-
Avoid straining while on the toilet.
|