The link between overall
health and oral health
September 13, 2004
The Australian Dental
Association Victorian branch (ADAVB) is urging the Australian public to pay
more attention to their oral health when visiting the dentist.
Dr Suzanne Hanlin, President of the ADAVB, says, “Australians should be
raising all their oral health issues, not just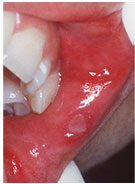 those related to teeth, with
their dentist. Oral Health is part of general health and disease often
appears first in the mouth, meaning oral health and disease should be
interlinked to general health and disease. Oral health conditions are often
best detected and managed by a dentist, and the ADA will be encouraging
Australians to discuss with their dentist symptoms such as unusual ulcers,
sores or lumps that don’t heal, symptoms of a dry mouth and bleeding gums
which might be indicative of other health conditions.”
those related to teeth, with
their dentist. Oral Health is part of general health and disease often
appears first in the mouth, meaning oral health and disease should be
interlinked to general health and disease. Oral health conditions are often
best detected and managed by a dentist, and the ADA will be encouraging
Australians to discuss with their dentist symptoms such as unusual ulcers,
sores or lumps that don’t heal, symptoms of a dry mouth and bleeding gums
which might be indicative of other health conditions.”
Research suggests that over a quarter of Australians have not visited their
dentist for three or more years. Conditions like oral cancer and diabetes
have a serious impact on an individual’s well being. They also impact on the
community in terms of social, emotional and financial burdens.
The ADAVB will be raising awareness of good oral health during August as
part of Dental Awareness Month. However, in 2004, the focus will move from
the teeth to include the whole mouth. In particular, the ADAVB will
highlight a number of very important oral health issues, including Oral
Cancer, Diabetes, Periodontal Disease linked to Cardiovascular Disease,
Ulcers, Eating Disorders, Dry Mouth Syndrome and Snoring.
Oral Cancers:
Oral cancers include cancers that affect the lips, tongue, cheeks, palate
and floor of the mouth. More deaths occur each year as a result of oral
cancer than cervical cancer. (Oral Health of Australians, Australian Health
Ministers’ Advisory Council, Steering Committee for National Planning for
Oral Health, August 2001.)
Oral cancers account for 6.5% of cancers diagnosed in Australia and account
for 2% of deaths. There is a link between oral cancer, alcohol consumption
and tobacco use, as well as sun exposure in the case of lip cancers. If oral
cancer is detected early, there is a 70% survival rate in the first 5 years,
compared to a 30% survival rate if the cancer has spread. (1998
December/Dental Update from a paper titled Orofacial Disease: Update for
Dental Clinical Team: 2. Ulcers, Erosions and Other causes if Sore Mouth
Part I, University of London.)
Importantly, research has found that the sufferers often ignore oral cancers
in their early stages. Regular oral tissue checkups conducted as part of a
routine dental visit can lead to early detection and treatment, meaning
better survival.
Diabetes:
With over one million Australians being affected by diabetes, the link
between the state of the mouth and diabetes becomes significant. A dentist
can play an important role in the detection of the early onset of diabetes
by alerting a patient to certain subtle signs and symptoms such as
non-responsive gum inflammation and persistent dry mouth. As well, people
diagnosed with diabetes must alert their dentist because of their increased
susceptibility to infection. “It is a cooperative relationship”, says Dr
Hanlin.
“We advise people to seek medical investigations for symptoms that might
indicate diabetes and the doctors advise their patients who have been
diagnosed with diabetes to seek regular dental inspections.” People who
suffer from symptoms of a burning mouth, dry mouth and altered taste should
also raise these symptoms when visiting their dentist as they may indicate
the onset of diabetes or poor control of diagnosed diabetes. Studies have
shown that 40% to 80% of people with diabetes suffer from a dry mouth, which
in turn has an association with increased dental cavities. (JADA, Vol. 132,
October 2001).
Periodontal disease linked to cardiovascular disease:
Periodontal disease, commonly known as gum disease often presents as
bleeding gums and low level inflammation, which can rapidly develop into
severe inflammation and eventually tooth loss.
Epidemiology studies indicate a link between oral diseases such as
Periodontal disease and systemic disease such as Cardiovascular disease.
While more Australians are keeping their teeth, this can increase the risk
of developing gum disease. With research suggesting a link between
Periodontal disease and Cardiovascular disease, the dentist’s role in
accurately diagnosing and treating Periodontal diseases becomes critically
important. Often the treatment goes beyond improved brushing and flossing
and may include specific treatment on the teeth to reduce the bacteria that
cause the disease. Australians need to be vigilant with proper brushing and
flossing which is shown to reduce the incidence of periodontal disease.
Ulcers:
Most people have experienced an ulcer, which is usually caused by some
trauma such as biting or burns to the lips or inside the mouth. Other very
common causes include denture rubbing or scratching from the broken corner
of a tooth.
Most ulcers heal within a week. However, if a person experiences an ulcer
that lasts longer than three weeks, they should visit their dentist for an
oral health check-up and specifically, analysis of the ulcer.
More uncommon causes of ulcers include some medications such as
anti-inflammatory, anti-diabetic and anti-malarial medicines. Additionally,
ulcers can be a sign of nutritional deficiencies, and in rare cases,
diseases such as Coeliac, Crohn’s disease and Ulcerative Colitis. It is also
not uncommon for people to develop ulcers related to menstruation, stress or
food allergies.
Very occasionally, an ulcer can represent early cancer, so persistent ulcers
need examination and the dentist is trained to recognise the cause, offer
treatment or refer the patient accordingly.
Eating disorders:
Conditions such as Anorexia Nervosa (accompanied by purging) and Bulimia can
often impact on oral health. Severe tooth damage and dental hypersensitivity
is not uncommon as vomiting brings stomach acids into the mouth, which in
turn leads to dental erosion. Dental erosion and hypersensitivity are often
permanent, which means lifelong management by the patient and the dentist is
necessary.
Additionally, symptoms such as dryness of the mouth due to a restricted diet
or recurrent vomiting can lead to increased dental cavities.
What is important is that sufferers establish a strong trust in their
dentist’s ability to continue to assist with managing these conditions.
Dry Mouth Syndrome: Also known as Xerostomia, Dry Mouth Syndrome is not a
disease, although it can be a symptom of certain diseases.
As its name implies, it refers to reduced saliva to the mouth, which leads
to a ‘dry’ mouth. It can produce serious negative effects on a person’s
quality of life, affecting dietary habits, nutritional status, speech,
taste, difficulty with dental prostheses such as dentures and increased
susceptibility to dental cavities. The increase in dental cavities can be
devastating in many patients and therefore special care must be made to
control this condition. Once again, the dentist is in the best position to
recognise and coordinate treatment for Xerostomia
Snoring and mouth breathers:
Snoring affects 7 million Australians and, along with sleep related
breathing disorders, it is one of the most common chronic health conditions.
While often thought of as a predominantly male condition, 30% of Australian
women also suffer from snoring, compared with 44% of men. Snoring is often
accompanied by a much more serious condition known as Sleep Apnoea, where
people stop breathing for abnormal periods during sleep. Dental patients
must tell their dentist about their snoring habits.
There are three classifications of Sleep Apnoea – central, obstructive and
mixed. Put simply, central sleep Apnoea refers to a situation where a
person’s airway is open, but they do not breathe. Obstructive sleep Apnoea
refers to the collapse of tissue around the airway during sleep, leading to
snoring as a result of breathing through a blocked airway. Mixed is a
combination of both.
The dentist is in the best position to discuss a range of treatment with
patients. These including referral to a Sleep Physician, alerting patients
to the positive effects of weight loss on snoring, changing sleeping
positions, restricting alcohol a few hours before sleep, avoiding of any
unnecessary use of sleeping tablets and taking care with over-the counter
drugs which might impact on sleep apnoea. More specific treatments for more
serious Sleep Apnoea in conjunction with the Sleep Physician include dental
appliances, Continuous Positive Airway Pressure and surgery.
The ADAVB urges all Australians to give consideration to their oral health,
and place importance on the raising any oral health issues with their
dentist. The ADAVB and its members are committed to improving the oral and
overall health of Australians and believe regular oral health examinations
by the dentist play a vital role in this.