|
|
Lasik Surgery
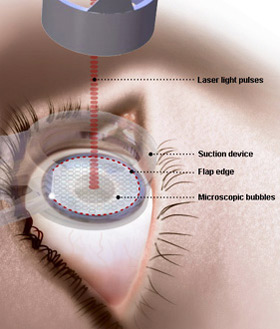 LASIK stands for �laser-assisted intrastromal in-situ keratomileusis,�
a vision correction procedure in which a flap of 160-180 microns depth is cut in
the front of the cornea, the flap is folded back to expose
the stroma of the cornea, an excimer laser ablates (reshapes) the exposed stroma,
and the flap is folded back down. LASIK stands for �laser-assisted intrastromal in-situ keratomileusis,�
a vision correction procedure in which a flap of 160-180 microns depth is cut in
the front of the cornea, the flap is folded back to expose
the stroma of the cornea, an excimer laser ablates (reshapes) the exposed stroma,
and the flap is folded back down.
The anterior layers of the cornea (epithelium, Bowman�s Layer) are preserved
(unlike in PRK, in which Bowman�s Layer is burned away by the laser and does not
grow back), and there is much less post-operative pain than with PRK, as well as
lower incidence of dry eyes, hazing, and scarring. Healing time is much faster
than for RK or PRK, and patients can see right away (I was seeing 20/25 the very
next day, and 20/20 a couple of days later). The surgery corrects myopia, hyperopia, and astigmatism, but cannot fix presbyopia. If you needed reading
glasses to see up close beforehand, you�ll still need them afterwards (unless
you opt for monovision, but you may still need the readers anyway).
Various essential steps in the direction of a safe & successful surgery are laid
down below. They are vital safeguards to make sure that you have a safe surgery
with the best possible chance of a good outcome.
-
Get your eyes screened you eye diseases, keratoconus, or retinal
problems, prior to the surgery (as all these problems disqualify you for
surgery).
-
Your surgeon will perform a cycoplegic refraction, in which he will give
you drops to paralyze your eyes� ability to accommodate, so that he can get
a very accurate refraction.
-
Cease to wearing soft contacts for at least one week prior to this exam,
and hard contacts for at least four weeks, and you may not wear them again
between the exam and your surgery (they can leave some residual
misshapenness in your cornea that can cause inaccurate surgery).
-
When you arrive at your laser center, a map, called a corneal
topography, will be made of your eye. This map will be used to help the
laser select a program, called a nomogram, to tell it how many pulses to
deliver to various spots on your cornea to produce the intended correction.
-
Your refractive error will be double-checked, possibly by using an
autorefractor, but definitely by hand with the phoropter (that funky
mask-shaped device your eye doctor uses to determine your prescription).
-
You
will be given drops to anesthetize your cornea, and measurements will be
made by tapping your cornea with a pachymeter to determine your corneal
thickness. You�ll see it, but you will not feel it. FYI, average corneal
thickness is about 500 microns at the center, tapering to about 300 microns
at the edges.
-
You will be given more numbing eye drops, and your face will be washed
with an antibiotic cleanser. You�ll also receive antibiotic eye drops and
either diazepam (the generic name for Valium) or iorezepam (the generic name
for Ativan) to help you calm your nerves. Make sure that you don�t take too
much of the medication, because you need to be awake during the procedure!
-
You will lie in the operating chair, which is motorized and will draw
you up under the operating microscope and laser. The eye that is not being
treated at the moment will be taped shut, and your operative eye will have
its lashes taped back with a surgical drape. You will be given much more
powerful anesthetic drops (usually Tetrocaine, a cocaine derivative). These
sting a little until they take effect. The surgeon will ask you if you can
still feel the stinging, and will continue to apply the drops until you
can't. Your cornea is very sensitive, so make sure you get all the
medication you need so that you feel nothing when your cornea is touched.
POST-OPERATIVE MANAGEMENT :
-
 After the procedure, you�ll suddenly feel heavy and sleepy, you will be
put in the waiting room for about 20 minutes for your corneas to bed down
some more, and may fall asleep. Your eyes will be checked under the slit
lamp microscope to verify that your flaps are properly bedded down, and then
you�ll be sent on your way, but you will NOT be allowed to drive, so make
sure you have someone with you. After the procedure, you�ll suddenly feel heavy and sleepy, you will be
put in the waiting room for about 20 minutes for your corneas to bed down
some more, and may fall asleep. Your eyes will be checked under the slit
lamp microscope to verify that your flaps are properly bedded down, and then
you�ll be sent on your way, but you will NOT be allowed to drive, so make
sure you have someone with you.
-
You will be asked to use a dark pair of wraparound sunglasses, every
time you go outside for the first week. Make it a point to use good
sunglasses regularly afterwards, since exposure to UV has been suspected in
causing haze in LASIK patients.
-
You will also be asked to use plastic eye shields that you should tape
over your eyes every night before going to sleep so that you don�t rub your
eyes and accidentally dislodge your flaps before the epithelium re-grows
over the edges.
-
The first 5 days are critical�you do not want to dislodge the flap!
After that critical period, you�re not going to move the flap without
surgical tools .
-
You will also be asked to make use of some steroid drops, some
antibiotic drops (ofloxacin is best), some artificial tears (patients in
Canada get this nifty tear gel instead), and possibly a non-steroidal
anti-inflammatory drop. Use them all religiously, and follow instructions.
-
Make sure you wash your hands before doing anything at all with your
eyes, so that the chance of infection is minimized. An infection under the
flap can cause scarring that can blind you, so do take extra care!
-
For about three months, you may experience fluctuations in your acuity.
You may see really well one day, and not so well the next. Be patient�
because there�s no blood supply, the cornea heals slowly. It can take three
to six months for vision to stabilize. Don�t even think about getting an
enhancement until at least three months have passed!
But can you ? Should you ? While many problems that dogged earlier
techniques have indeed been ironed out, many experts fear that the ads may be
misleading. Even the surgeons who perform the techniques admit that only about
half of all patients end up with 20/20 vision six months.
HOW BLIND ARE YOU?
 The acuity of your vision depends largely on the shape of your cornea, a
transparent cap that covers the iris and pupil. As light enters the eye, the
cornea helps focus the incoming image. If your cornea' s too steeply curved,
you're nearsighted -- distant object look blurry. Too flat and you're
farsighted, unable to sharply focus on people or object close at hand. If
you have an astigmatism, your cornea is steep and flat by turns. In
theory, at least, refractive surgery can eliminate all the flaws by slightly
changing the cornea's shape. The acuity of your vision depends largely on the shape of your cornea, a
transparent cap that covers the iris and pupil. As light enters the eye, the
cornea helps focus the incoming image. If your cornea' s too steeply curved,
you're nearsighted -- distant object look blurry. Too flat and you're
farsighted, unable to sharply focus on people or object close at hand. If
you have an astigmatism, your cornea is steep and flat by turns. In
theory, at least, refractive surgery can eliminate all the flaws by slightly
changing the cornea's shape.
But take note : If you're suddenly found yourself struggling to read the phone
book or thread a needle, chances are the lenses of your eyes have started to
stiffen, as happens in most adults by age 45. None of the surgical techniques
introduced thus far can eliminate the need for reading glasses.
In 1978 eye surgeons began to use a technique called Radical Keratotomy (RK
),which is essentially a series of incisions made around the iris to flatten the
cornea. That eased myopia, but the deep cuts were painful as they healed into
scars that often clouded vision. In 1987 Photorefractive Keratectomy ( PRK )
produced better results by using a laser to more lightly sculpt the cornea, but
haziness and discomfort often persisted.
The solution was LASIK, developed around 1990. LASIK skips scraping the top of
the cornea in favour of sculpting beneath its surface ; it's known as " flap and
zap " in surgery circles. The doctor first numbs the eye, then carefully slices
across the cornea a flap the thinness of an onion skin and hold it out of the
way. Next with the eye looking like a peeled grape, the laser goes to work
shaving off less sensitive cells underneath. After about a minute, the flap's
replaced, and the procedure's over. The flap re-adheres to the eye much like a
plastic warp. Recovery time's quicker than with PRK, and there's little pain ;
most people return to work in a day or two.
LASIK'S success rate is impressive, too -- at least in the hands of experienced
surgeons. Many are delivered with 20/ 20 vision, while another 20per cent get at
least 20/40. LASIK was initially built for just nearsighted patients. Today, the
procedure can help those who are mildly to moderately farsighted or who have an
astigmatism as well.
But every operation has a margin of error, and with LASIK the trickiest part
is creating the flap. If it's not quite right --too ragged, for instance
--and the surgeon goes ahead and does the lasering the eye won't heal "
correctly," and there may be scarring. To reduce the chance of a mishap, experts
advise patients to choose a highly experienced surgeon from a reputable hospital
who has enough humility to know when to call off the procedure.
Unfortunately, certain side affects aren't predictable and can never be undone
If the calibration of the laser is off --which can happen in the hands of even
the most skilled doctors -- you could go into the operating room nearsighted and
end up a bit farsighted, or vice versa. And about 5 percent of patients struggle
with chronic glare after LASIK, or see halos around bright lights. Such
complications, especially noticeable at night or while driving, can be a
nuisance for some people and a nightmare for others.
 you shouldn't consider LASIK if you have diabetes or any other medical condition
that threatens eyesight, or if your lens prescription has appreciably changed in
the previous five years The stronger your lens prescription, the higher the risk
of side effects ; there's simply more to be done in the eye. It also helps to
have a fat wallet: LASIK runs to about Rs.22,000 per eye and insurance companies
do not cover the cost. you shouldn't consider LASIK if you have diabetes or any other medical condition
that threatens eyesight, or if your lens prescription has appreciably changed in
the previous five years The stronger your lens prescription, the higher the risk
of side effects ; there's simply more to be done in the eye. It also helps to
have a fat wallet: LASIK runs to about Rs.22,000 per eye and insurance companies
do not cover the cost.
In the end, how satisfied you're likely to be with LASIK depends mostly on
how poor your vision is beforehand and bothersome you find contacts or glasses.
If even a mild improvement in vision would make you happy, you 're less likely
to be put off by the risks or common side effects.
Remember : No procedure can guarantee that you'll never wear glasses or contacts
again. Even at their most effective, LASIK just buy a little lens -free time.
Surgery or not, nearly everyone eventually needs glasses to read.
|
|
|
|
|









