|
|
Moles or Pigmented Nevi
 A
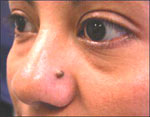
mole is a non-cancerous
skin growth made
up of cells (melanocytes or nevus cells) that produce color
(pigment). They can appear anywhere on the skin, alone or in groups.
Small A
mole is a non-cancerous
skin growth made
up of cells (melanocytes or nevus cells) that produce color
(pigment). They can appear anywhere on the skin, alone or in groups.
Small
in size (less than 5 mm), well-circumscribed lesion with
a well-defined border and a single shade of pigment from beige or
pink to dark brown. Most or all of the individual patient�s moles
often are similar to each other with respect to color and size.
Moles are usually present at birth or appear early in life. In time they may
grow larger. Although they may never make trouble aside from their
unsightliness, some of them may become
cancerous, spreading
cancerous cells through the bloodstream to other parts of the body.
The life cycle of an average mole is about 50 years. As the years pass, moles
usually change slowly, becoming raised and lighter in color. Often, hairs
develop on the mole. Some moles will not change at all. Some moles will slowly
disappear over time.
 What
causes a mole?
What
causes a mole?
Moles occur when cells in the
skin grow in a cluster instead of being spread throughout the skin.
These cells are called melanocytes, and they make the pigment that
gives skin its natural color. Moles may darken after exposure to the
sun, during the teen years and during
pregnancy.
A few of these moles, called congenital melanonaevi, are usually present at
birth. But most develop spontaneously or are caused by exposure to sunlight and
tend to appear on those areas of the skin that catch the most sunlight. Most of
these moles appear during the first 20 years of life, although they may continue
to develop into the 30s and 40s. However, the majority disappear with age.
 Types
of moles
Types
of moles
-
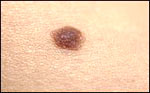 Congenital
Nevi: Moles that appear at birth. Congenital nevi
occur in about 1 in 100 people. These moles may be more likely to
develop into melanoma than are moles that appear after birth. If the
mole is more than 8 inches in diameter, it poses a significant risk
of becoming cancerous. Congenital
Nevi: Moles that appear at birth. Congenital nevi
occur in about 1 in 100 people. These moles may be more likely to
develop into melanoma than are moles that appear after birth. If the
mole is more than 8 inches in diameter, it poses a significant risk
of becoming cancerous.
-
Dysplastic Nevi: Moles that are larger than
average (larger than a pencil eraser) and irregular in shape. They tend to have
uneven color with dark brown centers and lighter, uneven edges. These moles tend
to be hereditary, and people with dysplastic nevi may have more than 100 moles.
People with dysplastic nevi have a greater chance of developing malignant
(cancerous) melanoma. Any changes in the mole should be checked by a
dermatologist to detect skin cancer.
-
Halo naevi: Occasionally the skin
surrounding a small mole becomes lighter and the central mole becomes pale. Most
halo naevi are benign. But some people may have an increased risk of developing
the skin disorder, vitiligo. Patients with malignant melanoma may, very rarely,
develop halo naevi.
-
Blue naevus: This deep-seated mole appears blue. It is very common
in some West Indian infants but is only rarely of any significance.
  Identifying
a malignant mole :
Identifying
a malignant mole :
The presence of moles is not a serious concern. but If there is a family history
of malignant melanoma, you should be particularly vigilant about changing moles.
-
The mole is itchy and painful.
-
Increased size or an increasingly irregular appearance, especially at the
edges.
-
A change in colour, particularly if the mole gets darker or becomes mottled.
-
Spontaneously bleeding.
-
Satellite pigmented lesions.
 Treating moles
Treating moles
To treat a mole, first a biopsy (small tissue
sample of the mole) is taken by a dermatologist so that thin sections of the
tissue can be examined under a microscope. This is a simple procedure. If the
dermatologist thinks the mole might be cancerous, cutting through the mole will
not cause the cancer to spread. If the mole is found to be cancerous, the
dermatologist will remove the entire mole.
There are two methods of removal:
-
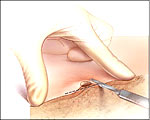 Shave excision (shaving it off)
Moles with an elevated surface typically are removed cosmetically by a
process called shave excision. This involves numbing the area around the
mole and removing the top portion of it so it is flush with the surrounding
skin. A small scar usually results, which is usually cosmetically
acceptable. If the mole had hair or was dark in color, these likely would
remain. There is a chance that after this procedure the mole could re-grow. Shave excision (shaving it off)
Moles with an elevated surface typically are removed cosmetically by a
process called shave excision. This involves numbing the area around the
mole and removing the top portion of it so it is flush with the surrounding
skin. A small scar usually results, which is usually cosmetically
acceptable. If the mole had hair or was dark in color, these likely would
remain. There is a chance that after this procedure the mole could re-grow.
The mole cells below the cut surface of the
removal site can also cause re-pigmentation of the removal site to a shade
much darker than that of the removed mole. This re-pigmentation side effect
is particularly problematic for patients with olive skin or dark eyes and
hair. Mole re-growth and re-pigmentation occur more commonly in young
patients and may result in the desire for re-removal.
-
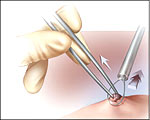
Elliptical excision
The cutting method of mole removal may be
used for both normal and atypical moles. (Potentially cancerous moles are
nearly always removed using this technique.) This procedure is often called
elliptical excision because the mole, as well as the surrounding and
underlying tissue, is removed in the shape of an ellipse, or oval. The
entire mole is removed, both above and below the skin. A small medical blade
may be used, or a laser may be chosen to reduce bleeding and allow for
quicker healing time. If a blade is used, sutures (stitched) are used to
close the incision if it is cut. If a laser is used, sutures will not be
needed. After the procedure, a bandage is usually applied.
-
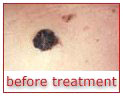 Laser treatment
Some moles can also be removed with lasers
instead of Laser treatment
Some moles can also be removed with lasers
instead of
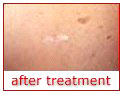 scalpels.
Because lasers seal blood vessels and evaporate the tissues they remove, the
need for cutting and sutures is eliminated. This may reduce scarring in some
cases. After laser surgery, a scab forms and falls off within 2 weeks. The
slight redness that is evident after the scab is gone will disappear in
time. scalpels.
Because lasers seal blood vessels and evaporate the tissues they remove, the
need for cutting and sutures is eliminated. This may reduce scarring in some
cases. After laser surgery, a scab forms and falls off within 2 weeks. The
slight redness that is evident after the scab is gone will disappear in
time.
If you see any signs of change in an existing
mole, if you have a new mole or if you want a mole to be removed for cosmetic
reasons, consult your dermatologist.
Who is an Ideal candidate for mole removal?
In general, the best candidates for mole removal are:
-
Fair skinned
-
Knowledgeable about the procedure
-
In good
physical and psychological health
-
Wanting to improve their appearance and/or
comfort
-
Realistic in their expectations
-
Not users of marijuana or anabolic steroids
-
Not heavy users of alcohol
The above is only a partial list of the
criteria that your surgeon will consider in determining whether or not this
procedure is appropriate for you. Be sure to ask your surgeon if he/she
considers you an ideal candidate for this surgery.
-
Tell your doctor about any allergies you have (to foods, drugs,
environmental elements)
-
Tell your doctor about all medications you are taking (both
prescription and non-prescription)
-
Carefully follow any instructions your doctor gives you.
|
Related Links
|
|
|
|
|









