|
|
CHORIOAMNIONITIS
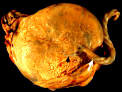 Chorioamnionitis
is an infection of two membranes of the placenta (the chorion and the amnion)
and the amniotic fluid that surrounds the baby. Chorioamnionitis can cause
bacteremia (blood infection) in the mother and may lead to preterm birth and
serious infection in the newborn baby. Other terms for chorioamnionitis include
intra-amniotic infection and amnionitis. Chorioamnionitis
is an infection of two membranes of the placenta (the chorion and the amnion)
and the amniotic fluid that surrounds the baby. Chorioamnionitis can cause
bacteremia (blood infection) in the mother and may lead to preterm birth and
serious infection in the newborn baby. Other terms for chorioamnionitis include
intra-amniotic infection and amnionitis.
The infection, which occurs in about 2 percent of all pregnancies, is caused by
bacteria that reach the uterus through the vagina.
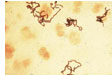 In
rare cases, chorioamnionitis occurs when there is no obvious rupture of the
membranes. In
rare cases, chorioamnionitis occurs when there is no obvious rupture of the
membranes.
The infection may be the cause of some cases of preterm labor.
For
this reason, doctors check first for infection in women who have preterm
labor.
The infection occasionally occurs early in pregnancy in women who have a
type of bacteria called beta streptococcus in their vagina.
Because this
bacteria can cause severe infections, such as pneumonia, in the newborn, a
doctor tests a woman's vaginal secretions to determine if beta streptococcus is
present.
If it is, the infection is treated immediately.
Signs/Symptoms
Symptoms of chorioamnionitis include fever and tenderness in the uterus. The
baby may show signs of infection, such as a fever or a higher-than-normal heart
rate.
Symptoms may include:
-
-
-
-
Tender or painful uterus
-
A foul odor of the amniotic fluid
-
The symptoms of chorioamnionitis may resemble other conditions or medical
problems. Always consult your physician for a diagnosis.
Risk of neonatal infection increases as the duration of ruptured membranes
lengthens. Chorioamnionitis may initiate uteroplacental bleeding or a placental abruption. Labor and delivery may be rapid in the presence of chorioamnionitis.
Alternatively, infection may cause uterine atony, requiring labor to be
augmented with Pitocin. Ultimately, a poor labor pattern may require an
instrumented delivery or a cesarean delivery. Each of these antepartum and
intrapartum factors must be considered when evaluating the newborn for the
presence of bacterial infection.
Diagnosis
In addition to a complete medical history and physical examination,
chorioamnionitis is diagnosed by symptoms and by laboratory tests for infection.
Testing of the amniotic fluid by amniocentesis may be needed.
 White blood cell (WBC) counts or C-reactive protein (CRP) levels in maternal
blood is commonly used to predict acute chorioamnionitis when maternal fever is
present. Different studies have supported or refuted the use of CRP to diagnose
chorioamnionitis. The CRP may be better than peripheral WBC counts in predicting
the risk of chorioamnionitis, especially if the mother has received
corticosteroids. Corticosteroids may falsely increase the total WBC count. White blood cell (WBC) counts or C-reactive protein (CRP) levels in maternal
blood is commonly used to predict acute chorioamnionitis when maternal fever is
present. Different studies have supported or refuted the use of CRP to diagnose
chorioamnionitis. The CRP may be better than peripheral WBC counts in predicting
the risk of chorioamnionitis, especially if the mother has received
corticosteroids. Corticosteroids may falsely increase the total WBC count.
Other investigators have suggested that the alpha1-proteinase inhibitor complex
in maternal blood is better than either CRP or WBC count to predict amniotic
fluid infection.
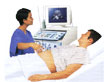 Ultrasonography may be used to ascertain fetal well-being. A biophysical profile
may provide information about the status of the fetus. Low biophysical profile
scores may be an indirect indicator of bacterial infection in the fetus. Imaging
has no direct means of indicating fetal infection with bacteria. Ultrasonography may be used to ascertain fetal well-being. A biophysical profile
may provide information about the status of the fetus. Low biophysical profile
scores may be an indirect indicator of bacterial infection in the fetus. Imaging
has no direct means of indicating fetal infection with bacteria.
Treatment
Specific treatment for chorioamnionitis will be determined by your physician
based on:
-
Your overall health and medical history
-
Extent of the condition
-
Your tolerance for specific medications, procedures, or therapies
-
Expectations for the course of the condition
-
Your opinion or preference
  The infection is treated with antibiotics, usually given intravenously in the
hospital. Because antibiotics given to woman do not reach the baby in quantities
sufficient to treat its infection, immediate delivery is recommended. If the
baby is born with severe infection, he or she is given antibiotics intravenously
to prevent or treat other infections - such as pneumonia or meningitis - that
can be caused by the same bacteria. The infection is treated with antibiotics, usually given intravenously in the
hospital. Because antibiotics given to woman do not reach the baby in quantities
sufficient to treat its infection, immediate delivery is recommended. If the
baby is born with severe infection, he or she is given antibiotics intravenously
to prevent or treat other infections - such as pneumonia or meningitis - that
can be caused by the same bacteria.
Diet
Seriously or critically ill newborns with early-onset bacterial infections
require parenteral fluids and nutrition until their condition improves.
Infections involving the GI tract may need a special approach to feeding when
feedings are reinstituted
Complications
For the mother with chorioamnionitis, serious infectious complications include
endometritis, localized pelvic infections requiring drainage, and
intra-abdominal infections. Maternal chorioamnionitis or other secondary
infectious complications may cause thrombosis of pelvic vessels and the
potential for pulmonary emboli.
Serious complications, including septic shock, pulmonary hypertension,
respiratory failure, and meningitis, do occur in early-onset bacterial
infections of the neonate. The duration of hospitalization can be quite
prolonged in an extremely premature infant because of infectious complications
such as maternal chorioamnionitis or congenital pneumonia. Either condition
increases the probability of chronic lung disease in prematurely born and term
babies.
Related Links
|
|
|
|
|









