|
|
Blepharospasm or Uncontrolled Flicker of the Eyelid
 The
term blepharospasm ['blef-a-ro-spaz-m] can be applied to any
abnormal blinking or eyelid tic or twitch resulting from any
cause, ranging from
dry eyes to Tourette's syndrome to tardive dyskinesia. It is
caused by a dysfunction of the area of the brain that controls
the muscles around the eye. Other
facial muscles can twitch as well, particularly those around
the cheek and brow. Severe cases can cause the eyelids to
forcibly close for a longer period than the typical blink,
disrupting vision. The
term blepharospasm ['blef-a-ro-spaz-m] can be applied to any
abnormal blinking or eyelid tic or twitch resulting from any
cause, ranging from
dry eyes to Tourette's syndrome to tardive dyskinesia. It is
caused by a dysfunction of the area of the brain that controls
the muscles around the eye. Other
facial muscles can twitch as well, particularly those around
the cheek and brow. Severe cases can cause the eyelids to
forcibly close for a longer period than the typical blink,
disrupting vision.
In the early stages it may only occur with specific
precipitating stressors, such as bright lights, fatigue, and
emotional tension. As the condition progresses, it occurs
frequently during the day. The spasms disappear in sleep, and
some people find that after a good night's sleep, the spasms
don't appear for several hours after waking.
Causes
Blepharospasm is thought to be due to abnormal functioning of the basal
ganglia which are situated at the base of the brain. The basal ganglia play
a role in all coordinated movements. It appears that there is a disturbance
of various "messenger" chemicals involved in transmitting information from
one nerve cell to another. In most people blepharospasm develops
spontaneously with no known precipitating factor.
It has been observed that the signs and symptoms of dry eye frequently
precede and/or occur concomitantly with blepharospasm. It
has been suggested that dry eye may trigger the onset of blepharospasm in
susceptible persons. Infrequently, it may be inherited. Blepharospasm can
occur with dystonia, a neurological movement disorder, in which sustained
muscle contractions might affect the mouth and/or jaw (oromandibular
dystonia, Meige syndrome). In such cases, spasms of the eyelids are
accompanied by jaw clenching or mouth opening, grimacing, and tongue
protrusion.
Blepharospasm can be induced by drugs, such as those used to treat
Parkinson's disease. Reducing the drug dose may alleviate the problem.
Symptoms occur most frequently in persons who are between the ages of 50 and
70. Women are three times more likely to develop the condition than men are.
The progression of symptoms includes:
- Spasms in response to particular triggers, such as fatigue or
bright lights
- Spasms occurring more frequently during the day, whether the
triggers are present or not
- Spasms forcing the eyelids shut for hours at a time � spasms
also pull the eyebrows down towards the eyes.
|
Treatment Options
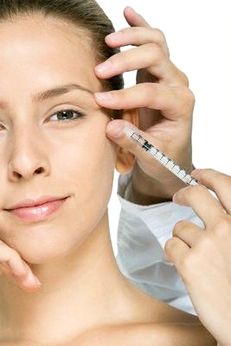 The
preferred treatment for many patients is the injection of
botulinum toxin (Botox).
Although the same bacterium responsible for botulism food
poisoning produces this toxin, it is safe in minute doses and
effective in stopping eyelid spasms. Botulinum toxin is injected
with a very fine needle into the eyelid, the brow, or the
muscles under the lower lid. It starts working in 1 to 14 days
and lasts an average of 3 to 4 months. Then the patient needs
another injection.
Click here to know about the dosages & number of injections
required to be administered. The
preferred treatment for many patients is the injection of
botulinum toxin (Botox).
Although the same bacterium responsible for botulism food
poisoning produces this toxin, it is safe in minute doses and
effective in stopping eyelid spasms. Botulinum toxin is injected
with a very fine needle into the eyelid, the brow, or the
muscles under the lower lid. It starts working in 1 to 14 days
and lasts an average of 3 to 4 months. Then the patient needs
another injection.
Click here to know about the dosages & number of injections
required to be administered.
Whether or not botulinum A toxin is working can be easily determined by
asking patients to squeeze the eyelids shut intensely and then try to
forcibly pry the eyelids open with the fingers. The patient with normal
squeezing requires significant force with the fingers to force the
eyelids open, whereas paralysis of the muscles of the eyelids allows the
eyelids to be opened easily. This simple test differentiates true
"failures of botulinum A toxin", in which the squeezing muscles are not
weakened by the toxin, versus those cases that have associated
deformities or problems.
|
Drug treatment for blepharospasm requires patience, as finding a
successful mix of drugs and doses may take some time. Some drugs (such as
lithium and diazepam (Valium)) are more effective for some patients than others,
and certain drugs may produce short-term benefits, unpleasant side effects or
both. It is important to follow the instructions of your ophthalmologist or
neurologist, and report side effects if they occur.
Functionally impaired patients with blepharospasm who have not tolerated or
responded well to medication or botulinum toxin are candidates for surgical
therapy. The principle is to stop contraction of an eye muscle called -
Orbicularis. At present, protractor myectomy (removal of some or all of the
muscles responsible for eyelid closure) has proven to be the most effective
surgical treatment for blepharospasm. Current experience has found that myectomy
has improved
visual disability in 75-80% of cases of blepharospasm. The first and easiest
group of patients to treat with myectomy surgery are those in whom botulinum A
toxin weakens the squeezing muscles, but have developed excess baggage in the
eyelids, stretching of the levator aponeurosis or tendon that raises the upper
eyelids (ptosis),
droopy brows, and on some occasions, mal-positions or in-turning or out-turning
of the eyelids and the lashes.
 Blepharospasm
symptoms tend to worsen in times of emotional stress. Learning
stress management techniques and joining a support group
can be helpful. Dark glasses are the commonest aid. They
fulfill two functions. They reduce the intensity of
sunlight which bothers many people with blepharospasm, and
they hide the eyes from curious onlookers. Lid hygiene to
decrease irritation and blepharitis should be encouraged.
Frequent applications of artificial tears and punctal occlusion
to alleviate dry eyes often improve symptoms. Blepharospasm
symptoms tend to worsen in times of emotional stress. Learning
stress management techniques and joining a support group
can be helpful. Dark glasses are the commonest aid. They
fulfill two functions. They reduce the intensity of
sunlight which bothers many people with blepharospasm, and
they hide the eyes from curious onlookers. Lid hygiene to
decrease irritation and blepharitis should be encouraged.
Frequent applications of artificial tears and punctal occlusion
to alleviate dry eyes often improve symptoms.
Join a support network. Sufferers have a fear of sustained attacks and feel
safer staying amongst familiar surroundings, putting them at risk of social
isolation.
Dated 13 February 2012
Related Links
|
|
|
|
|









