|
|
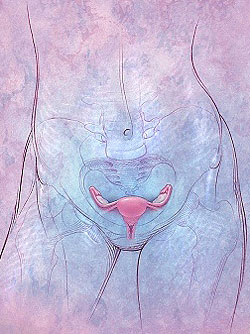
Uterine Fibroid Embolization (UFE)
UFE offers another route for treatment against uterine fibroids while
preserving the uterus.
Uterine
fibroids are also called fibromyomas, leiomyomas or myomas and usually
appear during an adult woman's childbearing years. Uterine fibroids are
noncancerous growths inside the uterus. They affect as many as three out of four
women sometime during their lives. Most times, there are no symptoms for the
fibroids. The fibroids are not associated with any increased risk of uterine
cancer nor are there cases where fibroids developed into cancer.
Uterine fibroid embolization (UFE) is a minimally invasive treatment for
fibroid tumors of the uterus.
In a UFE procedure, physicians use an x-ray camera called a fluoroscope to
guide the delivery of small particles to the uterus and fibroids. The small
particles are injected through a thin, flexible tube called a catheter. These
block the arteries that provide blood flow, causing the fibroids to shrink.
Nearly 90 percent of women with fibroids experience relief of their
symptoms.
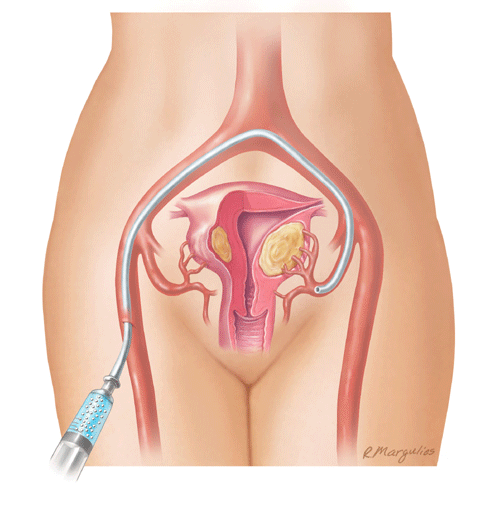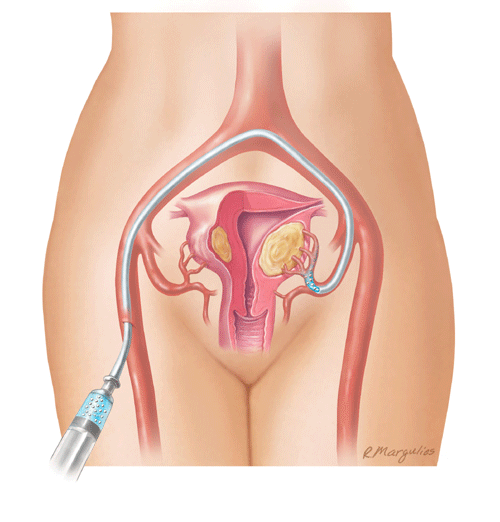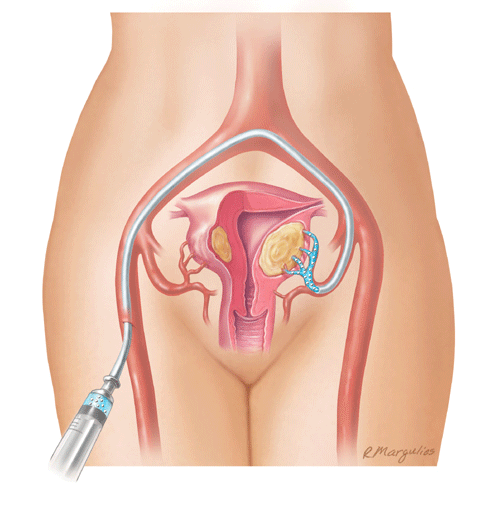
Note: Because the effect of uterine fibroid embolization on fertility is not
fully understood, UFE is typically offered to women who no longer wish to become
pregnant or who want or need to avoid having a hysterectomy, which is the
operation to remove the uterus.
You may be a candidate for uterine fibroid embolization (UFE), also known as
uterine artery embolization (UAE), if you fit into any of the following
categories:
-
Women who are experiencing the symptoms of uterine fibroids
-
Women who do not desire future
fertility
-
Women who want to retain their uterus, and so are pursuing hysterectomy
alternatives
-
Women who do not desire surgery
-
Women who may be poor surgical candidates; i.e.
obesity, bleeding disorders,
anemia
-
Women who are not pregnant
Once you have determined that you may be a candidate for uterine artery
embolization based upon the above criteria, then you will need some physician
input to help you decide how best to treat your uterine fibroids.
What are the benefits vs. risks?
Benefits
-
 Uterine fibroid embolization, done under
local anesthesia, is much less invasive than open surgery done to remove
uterine fibroids or the whole uterus (hysterectomy). Uterine fibroid embolization, done under
local anesthesia, is much less invasive than open surgery done to remove
uterine fibroids or the whole uterus (hysterectomy).
-
No surgical incision is needed�only a small
nick in the skin
that does not have to be stitched closed.
-
Patients ordinarily can resume their usual
activities weeks earlier than if they had a hysterectomy.
-
Blood loss during uterine fibroid
embolization is minimal, the recovery time is much shorter than for
hysterectomy, and general anesthesia is not required.
-
Follow-up studies have shown that nearly 90
percent of women who have their fibroids treated by uterine fibroid
embolization experience either significant or complete resolution of their
fibroid-related symptoms. This is true for women with heavy bleeding and for
those with bulk-related symptoms such as pelvic pain or pressure. On
average, fibroids will shrink to half their original volume, which amounts
to about a 20% reduction in their diameter.
-
Follow-up studies over several years have
shown that it is rare for treated fibroids to re-grow or for new fibroids to
develop after uterine fibroid embolization. This is because all fibroids
present in the uterus, even early-stage masses that may be too small to see
on imaging studies, are treated during the procedure. Uterine fibroid
embolization is a more permanent solution than another option,
hormone
therapy, because when hormonal treatment is stopped the fibroid tumors
usually grow back. Regrowth also has been a problem with laser treatment of
uterine fibroids.
Risks
-
Any procedure that involves placement of a
catheter inside a blood vessel carries certain risks. These risks include
damage to the blood vessel, bruising or bleeding at the puncture site, and
infection.
-
When performed by an experienced
interventional radiologist, the chance of any of these events occurring
during uterine fibroid embolization is less than one percent.
-
 Any procedure where the skin is penetrated
carries a risk of infection. The chance of infection requiring antibiotic
treatment appears to be less than one in 1,000. Any procedure where the skin is penetrated
carries a risk of infection. The chance of infection requiring antibiotic
treatment appears to be less than one in 1,000.
-
There is always a chance that an embolic
agent can lodge in the wrong place and deprive normal tissue of its oxygen
supply.
-
An occasional patient may have an allergic
reaction to the x-ray contrast material used during uterine fibroid
embolization. These episodes range from mild itching to severe reactions
that can affect a woman's breathing or blood pressure. Women undergoing UFE
are carefully monitored by a physician and a nurse during the procedure, so
that any allergic reaction can be detected immediately and addressed.
-
Approximately two to three percent of women
will pass small pieces of fibroid tissue after uterine fibroid embolization.
This occurs when fibroid tissue located near the lining of the uterus dies
and partially detaches. Women with this problem may require a procedure
called D & C (dilatation and curettage) to be
certain that all the material is removed so that bleeding and infection will
not develop.
-
In the majority of women undergoing uterine
fibroid embolization, normal menstrual cycles resume after the procedure.
However, in approximately one percent to five percent of women, menopause
occurs after uterine fibroid embolization. This appears to occur more
commonly in women who are older than 45 years.
-
Although the goal of uterine fibroid
embolization is to cure fibroid-related symptoms without surgery, some women
may eventually need to have a hysterectomy because of infection or
persistent symptoms. The likelihood of requiring hysterectomy after uterine
fibroid embolization is low�less than one percent.
-
Women are exposed to x-rays during uterine
fibroid embolization, but exposure levels usually are well below those where
adverse effects on the patient or future childbearing would be a concern.
-
The question of whether uterine fibroid
embolization impacts fertility has not yet been answered, although a number
of healthy pregnancies have been documented in women who have had the
procedure. Because of this uncertainty, physicians may recommend that a
woman who wishes to have more children consider surgical removal of the
individual tumors rather than uterine fibroid embolization. If this is not
possible, then UFE may still be the best option.
-
It is not possible to predict whether the
uterine wall is in any way weakened by UFE, which might pose a problem
during delivery. Therefore, the current recommendation is to use
contraception for six months after the procedure and to undergo a
Cesarean
section during delivery rather than to risk rupturing the wall of the uterus
during the contractions of labor.
Related Links
|
|
|
|
|









