
Lower Back Pain is a common and chronic problem . It can be caused and worsened by many different factors , including wrong exercise, lifting heavy
Objects with incorrect posture and pregnancy .If pain is intense see your doctor . He or she can rule out a serious condition such as herniated disc or broken bone in your back .
Low back pain affects 60 to 80 percent of the adult U.S. population at one time or another. Low back problems affect the spine’s flexibility, stability, and strength, which can cause pain, discomfort, and stiffness.
SIGNS AND SYMPTOMS
- Tenderness, pain and stiffness in the lower back
- Pain that radiates into the buttocks or legs
- Difficulty standing erect or standing in one position for a long time
- Discomfort while sitting
- Weakness and leg fatigue while walking.
Structure Of Normal Spine

TYPES OF LOWER BACK PAIN :
- Common types of low back pain for young adults (< 60 years old)
1. Muscle Strain :-
The majority of episodes of acute low back pain are due to a muscular strain (such as from lifting a heavy object or a sudden movement).
Muscle strains usually heal with time (a couple of days or weeks) because muscles have a good blood supply to bring the necessary nutrients and proteins for healing to take place.
2. Leg Pain And Possible Numbness :-
Pain that radiates through the buttocks, as well as pain and possibly numbness that radiates down to the foot, is frequently caused by a disc herniation in the lumbar (lower) spine. This type of pain is usually worse after a long period of standing or sitting.
3. Mechanical Low Back Pain :-
Low back pain in young adults that is caused by movement (such as bending forward, running) is commonly caused by a syndrome called degenerative disc disease. This condition can result from a twisting injury that weakens the disc. The low back pain symptoms of degenerative disc disease can become chronic and may tend to fluctuate and at times become significantly worse.
4. Low Back Pain (and possibly leg pain) that worsens when standing or walking :-
Sometimes a vertebral body in the low back slips forward, causing stress on the disc, which in turn may cause low back pain and may sometimes cause leg pain. These painful symptoms are sometimes caused by a stress fracture that occurs at a young age.
- Common types of low back pain for older adults (>60 years old)
1. Low Back Pain :-
That is worse in the morning and in the evening, and stiffness Low back pain that is most pronounced first thing in the morning and later in the day is often caused by facet joint osteoarthritis (degenerative arthritis), a condition that involves breakdown of the cartilage between the facet joints in the back. The pain and stiffness is a result of the lack of cartilage between the joints.
2. Pain down the legs when walking and standing upright :-
Leg pain that occurs when walking, and increases with more walking, can be caused by conditions such as lumbar spinal scoliosis or degenerative spondylolisthesis. Both conditions place pressure on the nerves at the point where they exit the spine. Standing upright, such as in normal walking, increases pressure on the nerve and results in leg pain.
WHAT CAUSES IT ?
Low back pain is usually caused by:
- Strain from lifting, twisting, or bending.
- However, some low back pain can be a symptom of a more serious condition, such as an infection, a rheumatic or arthritic condition, or ovarian cysts.
- It may be caused by a ruptured or bulging disk, the strong, spongy, gel filled cushions that lie between each vertebra.
- Compression fractures of the bones in the spine can also cause low back pain, specially in older women with osteoporosis.
- In addition, poor overall fitness, smoking, and general life dissatisfaction increase a person’s risk for low back problems.
TREATMENT & THERAPIES
Low back pain can often be relieved and prevented with lifestyle changes. Exercising to strengthen your muscles, maintaining a healthy weight, and practicing good posture lowers your risk. Physical therapy helps relieve pain for some people. For more severe or long-term back pain, your health provider may recommend medication or surgery.
REST
At the onset of lower back pain it is generally advisable to try one or two days of bed rest to decrease muscle spasm and allow the back to rest. More extensive bed rest seems to be counterproductive because it leads to further de-conditioning (weakening) of the muscles that provide critical support for the spine.
In addition to initial bed rest, either one or a combination of several conservative treatment options is often recommended in order to alleviate pain and rehabilitate the lower back.
DRUG THERAPIES
PRESCRIPTION
Muscle relaxants -for pain relief, especially at the onset of pain; various side effects . Typically, muscle relaxants are prescribed early in a course of back pain, on a short-term basis, to relieve low back pain associated with muscle spasms. There are several types of muscle relaxant medications that are commonly used to treat low back pain .
No steroidal anti-inflammatory drugs-used continuously for chronic pain; various side effects. NSAID’s work like aspirin by limiting the formation of inflammation, but have fewer gastrointestinal side effects (such as gastritis or ulcers) than aspirin
Oral or epidural steroids-reduce inflammation and can have dramatic results for pain relief, but have little lasting benefit; less effective with repeated use; various side effects. oral steroids are intended for use for short periods of time (one to two weeks). Oral steroids come in many forms, but are usually ordered as a Medrol Dose Pack in which patients starts with a high dose for initial low back pain relief and then taper down to a lower dose over five or six days.
OVER THE COUNTER
Aspirin or acetaminophen (Tylenol)- for pain relief; used continuously for chronic pain; various side effects. Acetaminophen is probably the single most effective non-prescription medication for lower back pain and has the fewest side affects. Tylenol is an example of a well-known medication that has acetaminophen as its active ingredient.
There are risks, side effects and drug interactions with any medication, so a medical professional should always be consulted prior to taking medications. Patients should be especially cautious with medications if they are on other medications or have any significant medical conditions (e.g. diabetes).
While a few major risks and side effects are outlined for some medications , patients should always read the label and package inserts and consult with a physician for a complete understanding of risks, side effects, and drug interactions. Drug detection services are available to ensure there are no adverse reactions between medications you’re taking and those already present in your body.
COMPLEMENTARY AND ALTERNATIVE THERAPIES
Alternative therapies can be effective for easing muscle tension, correcting spinal imbalances, relieving discomfort, and averting long-term back problems by improving muscle.
PHYSICAL THERAPY
After an episode of low back pain has lasted between two and six weeks, or if there are frequent recurrences of low back pain, it is reasonable to consider physical therapy for treatment. (Some spine specialists consider physical therapy sooner, particularly if the pain is severe.) In general, the goals of physical therapy are to decrease back pain, increase function, and provide education on a maintenance program to prevent further recurrences.
There are many different forms of physical therapy. Acutely, the therapist may focus on decreasing pain with passive physical therapy (modalities). These are considered passive therapies because they are done to the patient. Examples of modalities include
Heat/ice packs
Heat and/or ice are easily available and are the most commonly used type of modality. Each helps reduce muscle spasm and inflammation.
Some patients find more pain relief with heat and others with ice. The two may also be alternated. They are generally applied for 10-20 minutes once every two hours, and are more useful early on (the first few days) in the course of an episode of pain.
TENS units
A transcutaneous electrical nerve stimulator (TENS) unit uses electrical stimulation to modulate the sensation of low back pain by overriding the painful signals that are sent to the brain. A trial is usually done first, and if the patient experiences substantial pain relief, a TENS unit may be used at home for low back pain relief on a long-term basis.
Iontophoresis
Iontophoresis is a means of delivering steroids through the skin. The steroid is applied to the skin and then an electrical current is applied that causes it to migrate under the skin. The steroids then produce an anti-inflammatory effect in the general area that is causing pain. This modality is especially effective in relieving acute episodes of pain
Ultrasound
Ultrasound is a form of deep heating in which sound waves are applied to the skin and penetrate into the soft tissues. Ultrasound is especially useful in relieving acute episodes of pain and may enhance tissue healing
EXERCISES
In addition to passive therapies, active physical therapy (exercise) is also necessary to rehabilitate the spine. Generally, a patient’s exercise program should encompass a combination of the following:
- Stretching
- Strengthening/pain relief exercises
- Low-impact aerobic conditioning
Even patients with a very busy schedule should be able to maintain a moderate exercise regimen that encompasses stretching, strengthening, and aerobic conditioning.
Stretching
Almost everyone can benefit from stretching the soft tissues—the muscles, ligaments and tendons—around the spine. The spinal column and its contiguous muscles, ligaments and tendons are all designed to move, and limitations in this motion can accentuate pain .
Every individual who has suffered from low back pain should stretch their hamstring muscles once or twice daily. The hamstring muscles seem to play a key role in low back pain, as patients who have low back pain tend to have tight hamstrings, and patients with tight hamstrings tend to have low back pain. Simple hamstring stretching does not take much time, although it can be difficult to remember, especially if there is little or no pain. Therefore, hamstring stretching is best done at the same time every day so it becomes part of a person’s daily routine.
A hamstring stretching routine should include applying pressure to lengthen the hamstring muscle for 30-45 seconds at a time, one to two times each day. The pressure on the muscle should be applied evenly and bouncing should be avoided, since a bouncing motion will trigger a spasm response in the muscle being stretched. The hamstring muscle may be stretched in a number of different ways. Options for hamstring stretching, listed from most difficult to least difficult, include:
The most common technique is to simply bend forward at the waist, with legs relatively straight, and try to touch the toes and hold this position.
If this approach is not well tolerated, less strain is applied to the back by sitting on a chair and placing the legs straight out in front on another chair, then reaching forward to try to touch the toes. One leg at a time may be stretched.
One of the least stressful techniques is to lie on the floor and pull the leg up and straighten by holding onto a towel that is wrapped behind the foot. One leg at a time may be stretched.
Another less stressful option is to lie on the floor, with the buttocks against a wall, and place the foot up against the wall and then try to push the knee straight. One leg at a time may be stretched.
With time the hamstring muscle will gradually lengthen, reducing stress to the low back. Stretching should not be linked to other exercises, since those exercises may not be done on a daily basis. In order to make stretching a part of one’s daily regimen, it is best to stretch every morning when getting up and before going to bed. Think of it as good back hygiene.
Strengthening
There are two primary forms of exercise for strengthening and/or pain relief that tend to be used for specific conditions: McKenzie exercises and dynamic lumbar stabilization exercises. When appropriate, the two forms of physical therapy may also be combined. To strengthen the back muscles, 15-20 minutes of dynamic lumbar stabilization or other prescribed exercises should be done every other day .
1. McKenzie exercises :-
These exercises are named after a physical therapist in New Zealand who noted that extending the spine could reduce pain generated from the disc space. Theoretically, extension may also help reduce a herniated disc and reduce pressure on a nerve root.
For patients who are suffering from leg pain due to a disc herniation (a radiculopathy), extending the spine may help reduce the leg pain by “centralizing” the pain (moving the pain from the leg to the back). For most patients, back pain is usually more tolerable than leg pain, and if a patient is able to centralize the pain, they may be able to continue with conservative treatment and avoid a surgical discectomy.
When the pain is acute, the exercises should be done frequently (every one to two hours). Patients should also try to avoid flexing the spine (bending forward).
McKenzie exercises may also be helpful for those individuals who have back pain due to degenerative disc disease. While sitting or flexing forward can accentuate low back pain for patients with degenerative disc disease, extending the spine can serve to relieve the pressure on the disc.
Note that the opposite is true in elderly patients who have facet osteoarthritis and/or lumbar (extending the spine jams the facet joints on the back and increases pressure across the joints, so these patients will typically feel better sitting, and have more pain with extension).

2. Dynamic lumbar stabilization exercises :-
With this technique, the physical therapist first tries to find the patient’s “neutral” spine, or the position that allows the patient to feel most comfortable. The back muscles are then exercised to teach the spine how to stay in this position. This technique relies on proprioception, or the awareness of where ones joints are positioned. Performed on an ongoing basis, these exercises can help keep the back strong and well positioned.
These stabilization exercises may also be done in conjunction with McKenzie exercises. The McKenzie exercises serve to reduce back pain, and the stabilization exercises help strengthen the back. Stabilization exercises can be rather rigorous and therefore may not be well tolerated by all patients. It may be advisable for elderly patients or patients in significant pain to use other less strenuous means of physical therapy.

Low-impact aerobic conditioning
Low impact aerobics (such as walking, bicycling or swimming) should be done for 30-40 minutes three times weekly, on alternate days from the strengthening exercises. Reconditioning through low-impact aerobic exercise is very useful for both rehabilitation and maintenance of the lower back.
Aerobically conditioned patients will have fewer episodes of low back pain, and will experience less pain when an episode occurs. Well-conditioned patients are also more likely to stay functional (e.g. continue working and carry on with recreational activities), whereas those patients with chronic low back pain who choose not to work on aerobic conditioning should expect to experience the gradual loss of functional capabilities.
There are several types of aerobic exercise that are gentle on the back and, when done on a regular basis, highly effective in providing conditioning.
Walking. In general, walking is very gentle on the back, and walking two to three miles three times per week is very helpful for patients.
Stationary bicycling. If walking is painful, stationary bicycling is also effective and may be less stressful on the back.
Water therapy. Exercise in the water provides for effective conditioning while minimizing stress on the back (see also water therapy below).
Water therapy.Beginning aerobic exercises in the water has the added benefit of un weighting the spine, which allows for more mobilization with less pain for the patient. Sometimes as the therapy progresses, the patient may transition to land exercises.
Water therapy is especially useful for patients in too much pain to tolerate land exercises or for elderly patients. For patients who have osteoarthritis, especially for elderly patients, an ongoing water therapy and aerobics program may be the most effective treatment option
NUTRITION
B-complex:
B1 (50 to 100 mg), B2 (50 mg), B3 (25 mg); B5 (100 mg); B6 (50 to 100 mg); B12 (100 to 1,000 mcg), folate (400 mcg per day) all reduced with stress and pain.
Vitamin E :
(400 IU per day), Vitamin C (1,000 to 3,000 mg per day)
Calcium :
(1,500 to 2,000 mg) and magnesium (700 to 1,000 mg) to regulate muscle contraction and ease spasm.
Bromelain:
(250 to 500 mg three times per day on an empty stomach) anti-inflammatory, works especially well with turmeric
HOMEOPATHY
Some of the most common remedies for this condition are listed below.
- Aesculus for dull pain with muscle weakness.
- Arnica montana especially with pain as a result of trauma.
- Colocynthis for weakness and cramping in the small of the back.
- Gnaphalium for sciatica that alternates with numbness.
- Lycopodium for burning pain, especially with gas or bloating.
- Rhus toxicodendron for stiffness and pain in the small of the back.
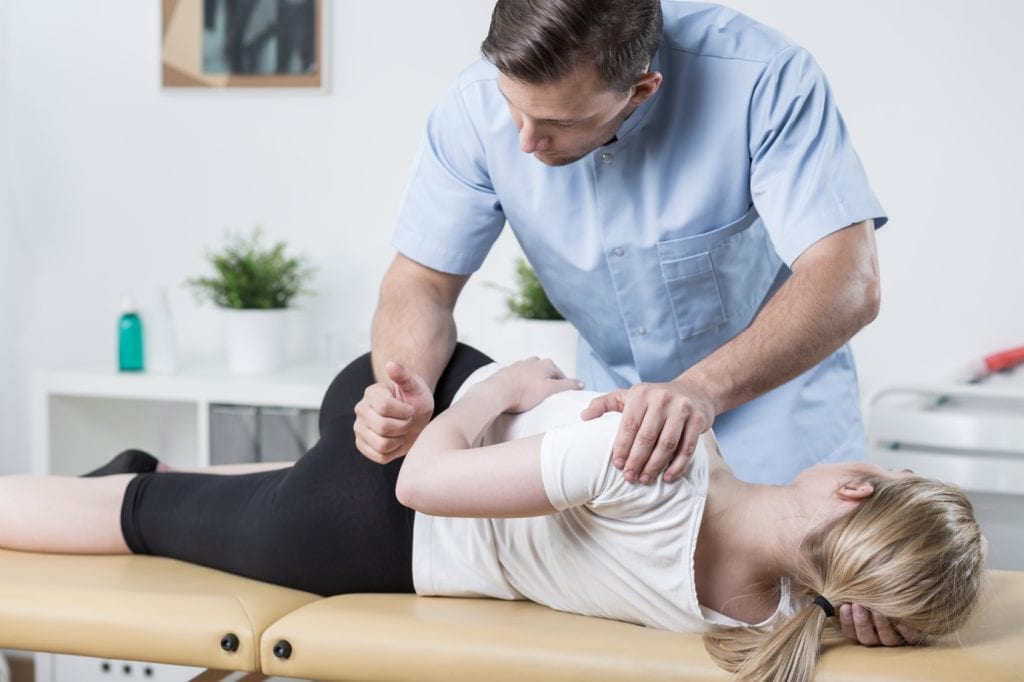
PHYSICAL MEDICINE
- Chiropractic or osteopedic manipulation can help relieve pain.
Chiropractic and osteopathic medicine represent another conservative treatment option for patients with low back pain. The overall philosophy for chiropractic and osteopathic manipulations is that joint dysfunction in the lower (lumbar) spine can produce low back pain. Mobilizing the lumbar spine joints though manipulations (commonly referred to as “adjustments”) can decrease low back pain.
Chiropractic or osteopathic manipulations can be especially helpful in relieving pain for facet joint injuries, osteoarthritis, and sacroiliac joint dysfunction, as these conditions represent joint dysfunction that responds well to mobilization.
- Contrast hydrotherapy.
Alternate hot and cold applications. Alternate three minutes hot with one minute cold. Repeat three times. This is done set. Do two to three sets per day.
- Castor oil pack.
Apply oil directly to skin, cover with a clean soft cloth and plastic wrap. Place a heat source over the pack and let sit for 30 to 60 minutes.
ACUPUNCTURE
May help relieve spasm and increase circulation to the affected area.
MASSAGE
Massage may be helpful both acutely and to prevent chronic problems.
SPECIAL CONSIDERATIONS
Chronic low back problems can interfere with everyday activities, sleep, and concentration. When symptoms are severe, your mood and sexuality may be affected. While depression is usually not the cause of chronic low back– pain, it often complicates treatment.
| For more: |
| The American Academy of Orthopaedic Surgeons has recommended a series of exercises that have been specifically chosen in order to help strengthen and condition the muscles that support the spinal column. Click here For more on back tools. Click here. |
Disclaimer
The Content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.




