How can I decide which is the best method of contraception for me?
There is no ideal, totally reliable and convenient method of contraception. Finding the method that will work best for you depends on many factors.
- How liable you are to side effects? The pill may not be advisable if you smoke or have high blood pressure. Some barrier methods can provoke cystitis.
- How important is avoiding pregnancy? Protection varies.
- Would the idea of an intrauterine device (IUD) trouble you? Would you mind taking artificial hormones every day?
- How regularly do you have sex? It it is occasional, condoms can be convenient.
- How much medical contact do you want? The pill, for example, requires regular visits.
- What method suits your personality? Not everyone can remember to take a daily pill.
Discuss these matters with your doctor or local family planning clinic. They will help you to decide what’s best for you, carry out fittings and supply you with whatever you need.
All forms of contraception are free on the NHS, and your local family planning clinic will supply free condoms.
The most common reason for failure of a contraception method is not using the method properly and consistently. Because of this, it’s recommended that you choose a method you feel comfortable using on a regular basis.

The most popular and effective contraceptive methods available around the world, include:
- Abstinence/Outercourse – is not having sexual intercourse. There are different ways to have sexual intercourse-sexual intercourse occurs when the penis enters the vagina, anus, or mouth. Outercourse is any kind of sexual activity in which the penis does not enter the vagina, mouth, or anus. It allows a couple to be more intimate and even have an orgasm with one another without having sexual intercourse. With outercourse, no semen, vaginal fluids, or blood is shared between partners. Abstinence and outercourse help prevent a person from getting or passing on sexually transmitted diseases-called STDs for short-which are diseases, infections, or illnesses that can spread from one person to another through sexual contact.
- Barrier methods – include condoms for males and females, diaphragms, and cervical caps. Male and Female Condoms are available “over the counter,” which means they can be bought at a store without a prescription. Your health care provider must prescribe the diaphragm and cervical cap. Barrier methods are placed either in the woman’s vagina or over a man’s erect penis (condoms) before having sex. The male latex condom protects against many sexually transmitted diseases-called STDs for short-which are diseases, infections, or illnesses that can spread from one person to another through sexual contact
- Fertility Awareness Based-Methods (FAB Methods) – A Fertility Awareness-Based (FAB) method (sometimes referred to as natural family planning) is a way for a woman to find out what days during her menstrual (monthly) cycle she either is or is not likely to get pregnant. The days she is likely to get pregnant are called “fertile” days. This is done by keeping track of the changes that occur in her body during the menstrual cycle-the time between the first day of her period and the last day before her next one. To avoid getting pregnant, a woman should not have sexual intercourse on her fertile days, unless she or her partner uses a barrier birth control method, such as a diaphragm or condom.
- Implants -(brand name Norplant®) are matchstick-size tubes placed in a woman’s upper arm just under her skin. They contain a hormone that prevents pregnancy for up to five years. However, implants can be removed at any time, and you then can become pregnant.
- Injectables -Injectables (brand name Depo-Provera®) are shots that contain progestin to prevent pregnancy. Women receive an injection in the buttocks or arm once every three months. The quarterly shot is similar to other progestin-only methods, such as mini-pills or implants, because it contains only one hormone.
- Intrauterine methods – Intrauterine devices (IUD) and intrauterine systems (IUS) are small, T-shaped pieces of plastic, which contain either copper or a hormone that prevents pregnancy (brand name Paragard® and Mirena®). Your health care provider puts the IUD or IUS in the uterus, also known as the womb, where it can remain for one to ten years, depending on your preference and the type you and your healthcare provider select
- Oral contraceptives (“the pill”)- Oral Contraceptives, also know as the pill, contain hormones that prevent pregnancy. Today’s pills are safe and effective for most women, if taken as prescribed.
- Spermicides – chemicals that kill sperm-include foams, creams, jellies, film, and suppositories. They are inserted deep into the vagina shortly before intercourse. Spermicides are also used with condoms. Some spermicides may help prevent sexually transmitted diseases
- Sterilization or Tubal ligation – is a procedure in which each of your fallopian tubes, the passageway from the ovary to the uterus, is blocked. This can be done by removing the tube, tying it off so an egg cannot get to the uterus, or placing an object in the tube that closes it. Female sterilization does not affect your sexual desire or attractiveness. During this procedure, no glands or organs will be removed or changed. After this procedure, all of your hormones will still be produced, your ovaries will still release an egg every month, and your menstrual cycle will most likely follow their regular pattern. Female sterilization is permanent; it is NOT reversible. You should consider possible changes in your life, such as divorce, remarriage, or death of children, in which case you may want to have children or more children.
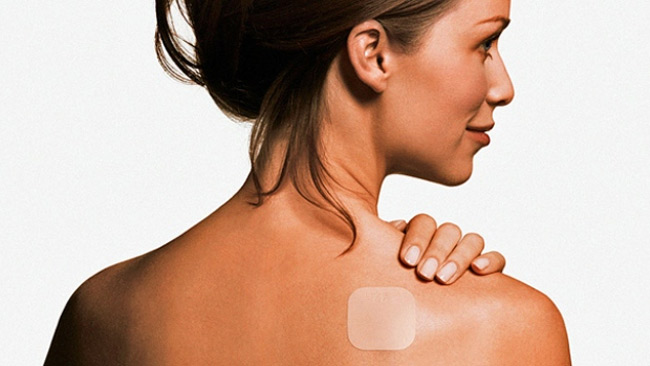
- Transdermal contraceptive patch (“the patch”) -The patch is a highly effective, weekly hormonal birth control patch that is worn on the skin to prevent pregnancy. It is worn for one week and replaced on the same day of the week for three consecutive weeks, with the fourth week “patch-free.” The patch is a very thin, beige, smooth square that measures 1-3/4 inch on each of its four sides. It uses a combination of the hormones estrogen and progestin to prevent pregnancy-like most birth control pills. It can be worn on the arms, buttocks, or abdomen. About 4 in 100 patches will partially or completely come off.
- Vaginal ring-
is a flexible ring worn in the vagina. It is folded and inserted high into the vagina, where it slowly releases estrogen and progestin. These hormones are absorbed into the bloodstream. Each ring is made of a type of vinyl and should be worn for three weeks out of the month. The ring is about two inches in diameter, and one size fits all women. - Vasectomy – is permanent birth control for men. The tubes in the scrotum that carry sperm to the penis can be either tied or sealed so no sperm are in the semen. Sperm are the reproductive cells in men, and semen is the fluid that carries sperm. Pregnancy can happen if a sperm joins with a woman’s egg. Vasectomy does not affect sexual desire or sexual performance. A vasectomy does not affect your ability to have and keep an erection or to ejaculate (or release sperm from the penis). The only difference is that the semen that is ejaculated no longer carries sperm. Your sperm will look just like it always did, and there will be about as much of it as before. Vasectomy is not effective immediately; sperm remain in the system beyond the blocked tubes. You must use other birth control until the sperm are used up. This usually takes from 15 to 20 ejaculations, or orgasms.
Each of these contraceptive methods has been proven safe if used properly. Please remember that using a combination of a male latex condom and other contraceptive methods can help prevent a person from getting or passing on sexually transmitted diseases-also called STDs for short-which are diseases, infections, or illnesses that can spread from one person to another through sexual contact. Some examples of STDs are chlamydia, herpes, HIV/AIDS, gonorrhea, and syphilis.
While some contraceptives have side effects, these can often be managed or relieved. Some methods, such as the pill, also offer many health benefits. The key to successful contraception is getting to know your birth control method
PROS AND CONS OF THE PILL
Taking the pill sounds so convenient, but I worry about the possible side effects. What are the short and long-term risks?
Many women who take the contraceptive pill notice very few side effects, or none at all. Women who take oestrogen-containing pills, however, may experience weight gain, nausea, vomiting, depression, water retention and headaches. Such effects usually disappear after a few months but, if they persist, it may be necessary to change to a different type of pill or to an alternative method of contraception. The higher the oestrogen content, the more likely such side effects are, so doctors tend to prescribe low-oestrogen pills wherever possible.
A more serious adverse effect of the pill is a greater tendency to blood clotting which can increase the risk of leg vein and lung thrombosis, and high blood pressure which increases the risks of heart disease or stroke. However, for non-smoking women under 35 years old the risk of any of these is tiny-about one in 77000. It increases with age, smoking and obesity, to about 1 in 500 for smokers over 45.
Oestrogen-containing pills are also associated with a slightly higher incidence of breast and cervical cancer (if condoms are not being used), especially among women who take them for long periods when very young and before having their first child. Oral contraceptives may also exacerbate or trigger conditions such as diabetes, heart disease or gallstones in women prone to these conditions.
On the positive side, the pill protects against cancer of the uterus and ovaries and against conditions such as rheumatoid arthritis and endometriosis. Used wisely and under medical supervision, it is a convenient, reliable and safe method of contraception for most women. Your doctor will advise you further.
Which pill is best?
- Low-dose pills have fewer side effects but are slightly less reliable.
- Every-day (ED) pills provide seven inactive pills instead of breaking your routine with pill-free days between packs.
- The minipill contains no oestrogen and is safer for some women.
- High-dose pills provide extra protection for very fertile women.
- Pills of different hormone content can help with problems such as acne or facial hair.
- Phasic pills which vary the hormone content are available for women who experience breakthrough bleeding with monophasic variety.
Contraceptive methods that won’t necessarily work

1. Breast feeding. While lactation may well turn off ovulation in some women most doctors recommend an additional form of contraception to be used as well if a pregnancy is really to be avoided.
2. Crossing one’s fingers
3. Intending to pull out
4. Words like ‘Just trust me, it’ll be OK’.
5. Douches/bidet. Beware! Sperm can swim against the tide.
6. Standing up during sex or jumping up and down afterwards
7. Cling wrap /chocolate wrappers… pleeeeease NO!
For more…. on family planning
Disclaimer
The Content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.