
- Structure of colon
- Risk Factors for colorectal cancer
- Symptoms of colorectal cancer
- Diagnosis
- Staging of Colorectal Cancer
- Treatment for colorectal cancer
The colon and the rectum are part of the large intestine, which is part of the digestive system. Because colon cancer and rectal cancers have many features in common, they are sometimes referred to together as colorectal cancer. Colorectal cancer includes cancers of both the large intestine (colon), the lower part of your digestive system, and the rectum, the last 8 to 10 inches of the colon.
Most colon and rectal cancers begin as small, noncancerous (benign) clumps of cells called adenomatous polyps. Over time some of these polyps become cancerous.
Structure of colon
The colon is the first 6 feet of the large intestine. It has four sections:
 |
- The first section is called the ascending colon. It extends upward on the right side of the abdomen.
- The second section is called the transverse colon since it goes across the body to the left side.
- There it joins the third section, the descending colon, which continues downward on the left side.
- The fourth section is known as the sigmoid colon because of its S-shape. The sigmoid colon joins the rectum, which, in turn, joins the anus, or the opening where waste matter passes out of the body.
Risk Factors for colorectal cancer
There are several causes for colorectal cancer as well as factors that place certain individuals at increased risk for the disease. There are known genetic and environmental factors.
People at risk for colorectal cancer:
- The biggest risk factor is age. Colorectal cancer is rare in those under 40 years. The rate of colorectal cancer detection begins to increase after age 40. Most colorectal cancer is diagnosed in those over 60 years.
- Have a mother, father, sister, or brother who developed colorectal cancer or polyps. When more than one family member has had colorectal cancer, the risk to other members may be three-to-four times higher of developing the disease. This higher risk may be due to an inherited gene.
- Have history of benign growths, such as polyps, that have been surgically removed.
- Have a prior history of colon or rectal cancer.
- Have disease or condition linked with increased risk.
- Have a diet high in fat and low in fiber.
Having certain diseases or conditions may place people at increased risk for colorectal cancer. These include
- Chronic ulcerative colitis, an inflammatory condition of the colon. People in this risk category have long-term disease, most for ten years or more.
- Crohn’s disease, which is an inflammatory disease of the gastrointestinal tract. This disease may increase colorectal cancer risk, although not as much ulcerative colitis.
- A history of breast, uterine, or ovarian cancer in women.
- Inherited a specific colorectal cancer syndrome. Those with an inherited syndromes may develop colorectal cancer at a much younger age, in their 30s or even younger. Over the past several years, genetic forms of colorectal cancer have been identified and genetic tests developed.
Symptoms of colorectal cancer
The symptoms of colorectal cancer can be confused with those of a number of digestive disorders. Having one or more of these symptoms does not mean you have cancer
The following are the most common symptoms of colorectal cancer. However, each individual may experience symptoms differently.
Women who have any of the following symptoms should check with their physicians, especially if they are over 40 years old or have a personal or family history of the disease:
- A change in bowel habits such as diarrhea, constipation, or narrowing of the stool that lasts for more than a few days.
- Rectal bleeding or blood in the stool
- Cramping or gnawing stomach pain
- Decreased appetite
- Vomiting
- Unexplained weight loss, unusually low red blood cell counts or anemia, weakness and fatigue
- Jaundice (yellowish coloring) of the skin or sclera of the eye
The symptoms of colorectal cancer may resemble other conditions, such as infections, hemorrhoids, and inflammatory bowel disease. It is also possible to have colon cancer and not have any symptoms. Always consult your physician for a diagnosis.
Diagnosis
Most colon cancers develop from polyps. Screening is extremely important for detecting polyps before they become cancerous. It can also help find colorectal cancer in its early stages when you have a good chance for recovery.
The doctor performs a thorough clinical evaluation that includes:
- A complete medical, family, and drug history
- A physical examination, including a digital rectal examination
Common screening and diagnostic procedures include the following:
- Digital rectal exam. In this office exam, your doctor uses a gloved finger to check the first few inches of your rectum for large polyps and cancers. Although safe and painless, the exam is limited to your lower rectum and can’t detect problems with your upper rectum and colon. In addition, it’s difficult for your doctor to feel small polyps.
- Fecal occult (hidden) blood test. This test checks a sample of your stool for blood. It can be performed in your doctor’s office, but you’re usually given a kit that explains how to take the sample at home. You then return the sample to a lab or your doctor’s office to be checked. The problem is that not all cancers bleed, and those that do often bleed intermittently. Furthermore, most polyps don’t bleed. This can result in a negative test result, even though you may have cancer. On the other hand, if blood shows up in your stool, it may be the result of hemorrhoids or an intestinal condition other than cancer. For these reasons, many doctors recommend other screening methods instead of, or in addition to, fecal occult blood tests.
- Flexible sigmoidoscopy. In this test, your doctor uses a flexible, slender and lighted tube to examine your rectum and sigmoid — approximately the last 2 feet of your colon. Nearly half of all colon cancers occur in this area. The test usually takes just a few minutes. It can sometimes be somewhat uncomfortable, and there’s a slight risk of perforating the colon wall.
- Barium enema. This diagnostic test allows your doctor to evaluate your entire large intestine with an X-ray. Barium, a contrast dye, is placed into your bowel in an enema form. During a double contrast barium enema, air is also added. The barium fills and coats the lining of the bowel, creating a clear silhouette of your rectum, colon and sometimes a small portion of your small intestine. This test typically takes about 20 minutes and can be somewhat uncomfortable. There’s also a slight risk of perforating the colon wall. A flexible sigmoidoscopy is often done in addition to the barium enema to aid in detecting small polyps that a barium enema X-ray may miss, especially in the lower bowel and rectum.
- Colonoscopy. This procedure is the most sensitive test for colorectal cancer and polyps. Colonoscopy is similar to flexible sigmoidoscopy, but the instrument used — a colonoscope, which is a long, flexible and slender tube attached to a video camera and monitor — allows your doctor to view your entire colon and rectum. If any polyps are found during the exam, your doctor may remove them immediately or take tissue samples (biopsies) for analysis. This is done through the colonoscope and is painless. If you have adenomatous polyps, especially those larger than 5 millimeters in diameter, you’ll need careful screening in the future.
A colonoscopy takes about a half-hour. You may receive a mild sedative to make you more comfortable. Preparation for the procedure involves drinking a large amount of fluid containing a laxative to clean out your colon — enemas are no longer necessary. Major risks of diagnostic colonoscopy include hemorrhage and perforation of the colon wall. But these risks are rare. Complications may be somewhat more frequent when polyps are removed.
- Genetic testing. If you have a family history of colorectal cancer, you may be a candidate for genetic testing. This blood test may help determine if you’re at increased risk of colon or rectal cancer, but it’s not without drawbacks. The results can be ambiguous, and the presence of a defective gene doesn’t necessarily mean you’ll develop cancer. Knowing you have a genetic predisposition can alert you to the need for regular screening. Still, you’ll also want to consider the psychological impact of what the test may reveal. Knowing you may develop cancer affects not only your own life, but the lives of everyone close to you. Genetic testing for children is even more complex and problematic. It’s best if you discuss all of the ramifications of genetic testing with your doctor or a medical geneticist.
Another new test checks a stool sample for DNA from abnormal cells. In preliminary studies, the test has proved to be so accurate it may eventually eliminate the need for more-invasive examinations such as colonoscopy, at least in average-risk circumstances. A three-year clinical trial of this test by the National Cancer Institute is under way.
| Screening Guidelines for Colorectal Cancer Colorectal cancer screening guidelines from the American Cancer Society for early detection include:Beginning at age 50, both men and women should follow this testing schedule: Digital rectal examination should be performed at the time of each screening sigmoidoscopy, colonoscopy, or barium enema examination. Yearly fecal occult blood test, plus: flexible sigmoidoscopy every 5 years, or colonoscopy every 10 years, or double contrast barium enema every 5-10 years People with any of the following colorectal cancer risk factors should begin screening procedures at an earlier age: strong family history of colorectal cancer or polyps (cancer or polyps in a first degree relative younger than 60 or in two first degree relatives of any age) family with hereditary colorectal cancer syndromes (familial adenomatous polyposis and hereditary non-polyposis colon cancer) personal history of colorectal cancer or adenomatous polyps personal history of chronic inflammatory bowel disease |
Staging of Colorectal Cancer
Staging is the process of finding out how far the cancer has spread. This is very important because your treatment and the outlook for your recovery depend on the stage of your cancer. For early cancer, surgery may be all that is needed. For more advanced cancer, other treatments such as chemotherapy or radiation therapy may be used.
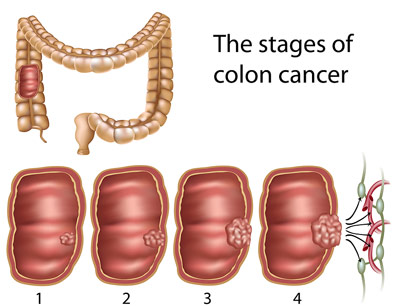
Stage 0
For cancers that are stage 0, the disease has not grown beyond the lining of the colon or rectum. Therefore surgical removal or destruction of the cancer is all that is needed. For larger tumors, a rectal or colon resection may be required.
Stage 1
For colon cancer, Stage 1 cancers have grown through several layers of the colon but have not spread outside the colon itself. Standard treatment is a colon resection with no other treatment generally needed.
Like colon cancer, Stage 1 rectal cancers have grown through numerous layers of tissue but not outside the rectum. The type of surgery used to treat this is dependant upon the location of the cancer, but the primary treatment is an abdominoperineal resection. Chemotherapy and radiation are sometimes administered before or after surgery.
Stage 2
Stage 2 colon cancer has penetrated the wall of the colon and spread into nearby tissue. However, it has not yet reached the lymph nodes. Usually the only treatment for this stage is a resection. Since some Stage 2 colon cancers have a tendency to recur, the doctor may also decide to treat the patient with chemotherapy or radiation therapy.
Once rectal cancer has reached Stage 2, it too has penetrated the walls of the rectum but has not yet reached the lymph nodes. It is generally treated with a resection and then both chemotherapy and radiation therapy.
Stage 3
Stage 3 is considered an advanced stage of colorectal cancer. The disease has spread to the lymph nodes, but not to other parts or organs in the body. For both colon and rectal cancer, sectional surgery is done first and is followed by chemotherapy and radiation therapy.
Stage 4
For patients with Stage 4 colorectal cancer, the disease has spread to distant organs such as the liver, lungs and ovaries. When the cancer has reached this stage, surgery is generally aimed at relieving or preventing complications as opposed to curing the patient of the disease. Occasionally the cancer’s spread is restricted enough to where it can all be removed by surgery. For Stage 4 cancer that cannot be surgically removed, chemotherapy, radiation therapy or both may be used to alleviate, delay or prevent symptoms
Treatment for colorectal cancer
Specific treatment for colorectal cancer will be determined by your physician based on:
- your age, overall health, and medical history
- extent of the disease
- your tolerance for specific medications, procedures, or therapies
- expectations for the course of the disease
- your opinion or preference
Treatment choices for the person with colon cancer depend on the stage of the tumor – if it has spread and how far. When the disease has been found and staged, your physician will suggest a treatment plan. Treatment may include:
- Colon surgery
Often, the primary treatment for colorectal cancer is an operation called a segmental resection, in which the cancer and a length of normal tissue on either side of the cancer are removed, as well as the nearby lymph nodes. - Radiation therapy
Radiation therapy is the use of high-energy radiation to kill cancer cells either after surgery, to kill small areas of cancer that may not be seen during surgery, or instead of surgery. Radiation may also be used to ease (palliate) symptoms such as pain, bleeding, or blockage. There are two ways to deliver radiation therapy, including the following: - External beam radiation
External beam radiation uses radiation from outside the body, which is focused on the cancer. - Internal radiation therapy
Internal radiation therapy uses small pellets of radioactive material placed directly into the cancer. - Chemotherapy
Drugs (medications) are given into a vein or by mouth to kill cancer cells throughout the body. Studies have shown that chemotherapy after surgery can increase the survival rate for patients with some stages of colon cancer. Chemotherapy can also help relieve symptoms of advanced cancer.
Disclaimer
The Content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.