Maybe you have heard the term, “pelvic floor” bandied about, but what exactly is that? With a range of issues that may be dramatically impacting your daily life such as incontinence, painful intercourse (dysparunia), overactive bladder, or even constipation, your pelvic floor may be the culprit. You might be surprised to learn that physical therapy is a first-line treatment for these and many other concerns. These issues, while common, should not be accepted as normal or untreatable.
I turned to Nancy Hughes, MPT, CLT a physical therapist from Southern New Hampshire Medical Center with over 20 years of experience assessing and treating a multitude of pelvic floor concerns to shed some light on this often overlooked area in women’s health.

Nancy Hughes, MPT, CLT a physical therapist from Southern New Hampshire Medical Center answers frequently asked concerns by women in close interaction with Charlene Bazarian
*When we are talking about the “pelvic floor,” what exactly are we talking about?
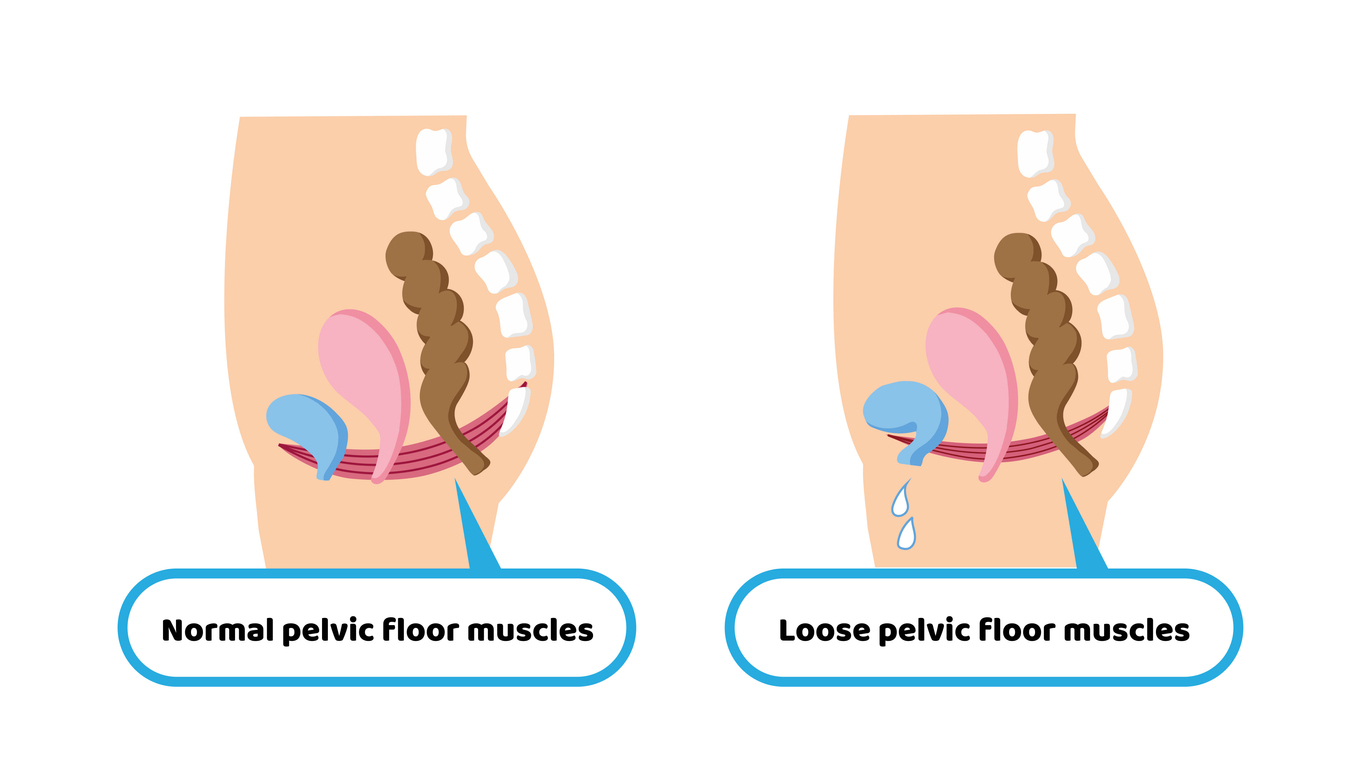
The pelvic floor refers to a group of muscles that line the lower portion of our pelvis. I like to describe the function of the pelvic floor as being similar to the architecture of a house. A solid house requires a roof, walls, and a floor. In this analogy, the roof or ceiling would be your diaphragm, the walls would refer to your abdominal wall and back muscles, and the floor would be the pelvic muscles. It is important for all of these muscles to work collectively to establish a strong, functional core. I personally would love to see women learn about their pelvic floor in adolescence because it plays such an important role in our overall health and well-being across our lifespan.
*How does physical therapy play a role in treating disorders of the pelvic floor?
First, it’s important to understand that these muscles are under our volitional control. Just like other muscles, such as your biceps or quadriceps, these are muscles you can contract and relax. The challenge for many is that you can’t see these muscles, thereby making it more difficult to be sure you are contracting or relaxing them correctly. A pelvic floor physical therapist will assess your functional ability to engage these muscles and teach you how to correctly perform the exercises to improve their strengths and extensibility. I explain to my patients that these muscles have several roles for sphincteric control, postural support to their pelvic organs, and sexual intimacy. I often joke that the bicep flexes my shoulder and bends my elbow but we know so much more about that than this group of muscles that have so many jobs to fill!
Additionally, a pelvic floor therapist will discuss nutrition/hydration, the physiology of voiding as it relates to the pelvic floor, and behavioral mechanisms that may be impacting some of the symptoms that women are experiencing.
*What kind of advice would you offer to women to help prioritize and improve the health of their pelvic floor?
My advice would vary according, in part, to the age of the individual. For women in their twenties and thirties, this would be generally considered to be prime child-bearing years. As such, regularly working on strengthening, as well as relaxation of the pelvic floor, is key to improved comfort during the prenatal period as well as improving the ease with delivery and subsequent postpartum recovery. While this may be in part, a classic kegel exercise, a pelvic floor physical therapist could more specifically guide you into the appropriate dosing of these and other exercises, diaphragmatic breathing, and how to relax the pelvic floor.
For women in their forties and fifties, we’re looking at the onset of perimenopause into menopause, and what’s significant at this time, is the role that estrogen plays in our continence. As estrogen declines, the wall of the urethra thins, thereby creating a more patent opening for urine to leak out. As a result, pelvic floor strength and integrity are even more vital to maintaining our continence. It is usual at this age that women make the incorrect assumption that this is just the way life proceeds for women. This is absolutely not the case and a qualified physical therapist well-versed in pelvic floor treatment can help to “right the ship” to a more normal physiologic function.
For those women in their sixties and beyond, while strength continues to be important, other issues we consider relate to problems stemming from dehydration and vaginal dryness. It is important to assess dietary intake as well as the quality of the vaginal tissue to further maintain the health of the pelvic floor. Oftentimes, as we age, hydration is something we become less aware of, which can further worsen issues like incontinence and constipation.
*How do you know when it is time to ask for help and seek treatment from a pelvic floor physical therapist?

If you are experiencing episodic urinary leakage, no matter how small, vaginal pain with or without penetration, difficulty with voiding urine, or emptying your bowels, then it’s time to ask your doctor for a referral to a qualified pelvic floor physical therapist. I understand how difficult these conversations can be to have, but in this day in age, we must advocate for ourselves when it comes to our health, no matter the issue. No symptoms that are impacting your daily life should be left untreated, particularly when non-surgical or non-pharmaceutical help is available.
Given all that physical therapy has to offer in this realm, let’s end the stigma that this is something you have to accept and live with. Trust me, I will talk about pee, poop, or sex with any anyone if I feel it will help improve their quality of life. So ladies, let’s build a strong foundation from the floor up!
For more about Nancy Hughes or if you live in the New England area, click here: Nancy Hughes – Southern New Hampshire Health (snhhealth.org)
About the author: Charlene Bazarian is a fitness and weight loss success story after losing 100 pounds. She mixes her no-nonsense style of fitness advice with humor on her blog at Fbjfit.com and on Facebook at FBJ Fit.
Disclaimer
The Content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.