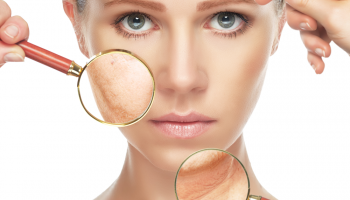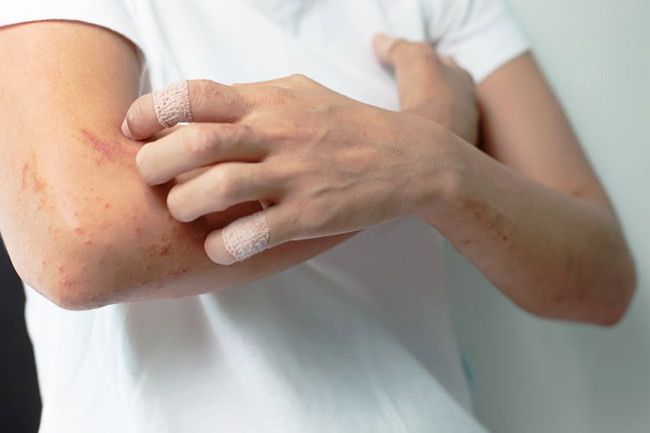
Shingles is a skin rash caused by the same virus that causes chickenpox. The virus responsible for these conditions is called Varicella zoster. After an individual has chickenpox, this virus lives in the nerves and is never fully cleared from the body. Under certain circumstances, such as emotional stress, immune deficiency (from AIDS or chemotherapy) or with cancer, the virus re-activates causing shingles.
Causes
Shingles is a second eruption of the varicella-zoster virus – the same virus that causes chickenpox.
Varicella-zoster is part of a group of viruses called herpes viruses, which includes the viruses that cause cold sores and genital herpes. Many of these viruses can lie hidden in your nervous system after an initial infection and remain inactive for years before causing another infection.
Anyone who’s had chickenpox may develop shingles. If your immune system doesn’t destroy the entire virus during the initial infection, the remaining virus can enter your nervous system and lie hidden for years. Eventually, it may reactivate and travel along nerve pathways to your skin – producing the shingles. However, it’s most common in older adults: More than half the shingles cases occur in adults over 60.
A person with shingles can pass the varicella-zoster virus to anyone who hasn’t had chickenpox before. This usually occurs through direct contact with the open sores of the shingles rash. Once infected, the person will develop chickenpox, however, not shingles. The infection can be serious for certain groups of people with immune system deficiencies. The varicella-zoster virus cannot be spread to another person with a normal immune system who has already had chickenpox.
Symptoms
- The first symptom of shingles is often extreme sensitivity or pain in a broad band on
one side of the body. The sensation can be itching, tingling, burning, constant aching, or deep, shooting, or “lightning bolt” pain. - Typically, 1-3 days after the pain starts, a rash with raised, red bumps and blisters erupts on the skin in the same distribution as the pain. They become pus-filled, then form scabs by 10-12 days.
- Fever and chills
- Headache
- Upset stomach or abdominal pain
- The rash disappears as the scabs fall off in the next 2-3 weeks, and scarring may result.
For some, pain can be intense, with just the slightest touch causing severe pain. Sometimes the pain can be mistaken for other problems or diseases, such as kidney stones, gallstones or appendicitis, depending on its location. Some people experience the pain without the rash, which makes diagnosing shingles more difficult.
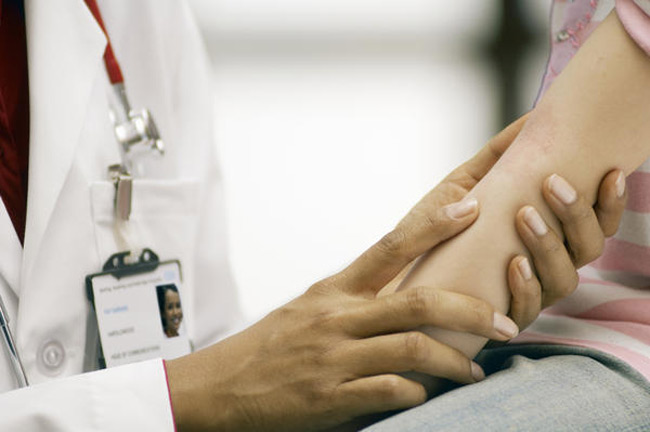
Although the shingles rash may resemble chickenpox, the virus typically causes more pain and less itching the second time around.
Diagnosis
Before the shingles rash appears, diagnosis of this condition may be difficult. Symptoms of shingles can mimic other conditions. The initial symptoms may include itching, numbness, tingling, or pain on one side of the body or face. During this stage, the pain may be so severe that it may be mistaken for kidney stones, pleurisy, gallstones, appendicitis, or even a heart attack depending on where the affected nerve is located on the body.
Your doctor can distinguish shingles from chicken pox, poison ivy, or other types of rash by the way the lesions are distributed on the body. The blisters of the shingles rash generally appear in the pattern of a band (dermatome) on one side of the body.
In addition to looking at how the rash appears on your body, your doctor may also take a scraping or swab of the blisters to send to a laboratory for analysis, beyond which, no further test will be required.
Treatment
The goals of treatment for shingles are to:
- Shorten the duration of the eruptive stage or rash
- Speed up healing of the lesions
- Relieve patient discomfort
- Shorten the duration of postherpetic neuralgia (PHN) or pain associated with shingles even after the rash is healed.

There is no cure for shingles, but treatment may shorten the length of illness and prevent complications. Treatment options include:
- Antiviral medicines, sometimes in combination with corticosteroids, to reduce the pain and duration of shingles.
- Pain medicines, antidepressants, and topical creams to relieve long-term pain.
Topical creams containing capsaicin may provide some relief from pain. Capsaicin may irritate or burn the skin of some people, and it should be used with caution. A new skin patch containing a 5% lidocaine solution is the only prescription medication approved by the Food and Drug Administration specifically for the treatment of the pain associated with PHN. However, patients with severe PHN may be ordered a nerve block through transcutaneous electrical nerve stimulation (TENS), which involves sending electrical impulses to the affected nerves to block the pain sensation.
Things you can do to promote healing of the shingles rash and reduce the pain:
- Apply cool compresses over the zoster lesions or take a cool bath twice a day
- Avoid exposure to warm and hot water because this could lead to further itching
- Cover shingles lesions with a clean cloth or loose-fitting gauze after cleansing
- Trim fingernails to reduce the chance of bacterial infection from scratching
- Avoid wearing tight clothing over the rash because this could irritate the rash
Prevention
The U.S. Food and Drug Administration (FDA) has approved a vaccine that may help prevent shingles or make it less painful if you do get it. The shingles vaccine is known as Zostavax. One dose is recommended for adults 60 years of age and older. Ask your doctor about the availability of this vaccine. Zostavax has not been studied in people who have already had shingles. It’s not known if the vaccine will prevent shingles from occurring again. The U.S. Food and Drug Administration (FDA) does not recommend this vaccine for people who have already had shingles.
If you have never had chickenpox, you may avoid getting the virus that causes both chickenpox and later shingles by receiving the varicella vaccine.
Disclaimer
The Content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.