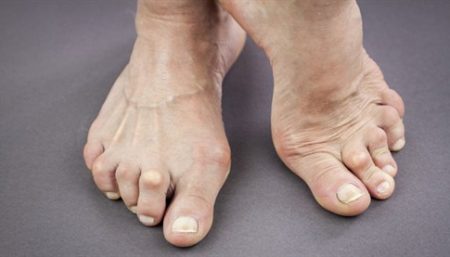
A fungal infection of the foot that produces cracked, sore, itchy skin between the toes.
Most common in teenagers and young adults.
Athlete’s foot, also called tinea pedis, is a common, persistent fungal infection of the feet that particularly affects the skin between the toes. The condition can be caused by several types of fungi that thrive in warm, humid conditions. A foot inside a shoe is the perfect place for the fungus.

 What are the Causes?
What are the Causes?
Athlete’s foot often affects teenagers and young adults, who tend to sweat more and wear enclosed footwear, such as trainers, for long periods. It is rare in children. Athlete’s foot can be picked up by walking barefoot in communal areas that are warm and humid, such as changing rooms and poolside.
Sweaty feet, tight shoes/socks, not drying one’s feet well after swimming, bathing, or exercising all contribute to the development of athlete’s foot.
 What are the Symptoms?
What are the Symptoms?
Athlete’s foot most commonly occurs between the fourth and fifth toes and produces the following symptoms:
- Cracked, sore, and itchy areas of skin.
- Flaking, white, soggy skin.
- In some people the skin becomes very sore and even bleeds a little.
- Athletes foot may also produce itching and burning of the feet.
Some times, the infection spreads on to the sole or the sides of the foot or affects the toenails, which then become yellowish, thickened, and brittle. Toenail infections cause scaling, crumbling, thickening, and even partial loss of the nails. These changes can also result from other conditions such as psoriasis, injury, and aging. Untreated, athlete’s foot can result in blisters and cracks that may lead to secondary bacterial infections.
People who have athlete’s foot are more susceptible to ringworm of the groin, another fungal infection. Those with acute tinea infections may develop similar outbreaks on their hands, typically on the palms. This trichophyde reaction, also known as tineas manuum, is an immune system response to fungal antigens (antibodies that fight the fungal infection).
 Diagnosis
Diagnosis
Diagnosis is made by visual observation of the symptoms. The podiatrist eliminates the possibility of a bacterial infection by performing a microscopic examination of skin scrapings to determine the type of fungus causing the infection. Other tests include growing a fungal culture from skin scrapings and examining the patient’s foot under an ultraviolet light.
 Treatment Options
Treatment Options
The affected area can be treated using an over-the-counter antifungal preparation available in form of creams, powders, and sprays, which should be applied at least twice a day .It is important that you continue to apply the preparation to affected areas for a few days after the symptoms have cleared up to make sure that the infection is eradicated.
available in form of creams, powders, and sprays, which should be applied at least twice a day .It is important that you continue to apply the preparation to affected areas for a few days after the symptoms have cleared up to make sure that the infection is eradicated.
If over – the – counter preparations do not help or you are unsure of the diagnosis, consult your doctor, who can give you further advice about treatment or prescribe aantifungal drug. The most effective chemical treatments these days are the imidazoles, eg miconazole and clotrimazole. If the infection becomes systemic, stronger antifungal medication may be prescribed. These drugs include griseofulvin (Fulvicin® and Grisactin®) and concentrated forms of terbinafine and itraconazole. Griseofulvin can cause side effects such as headache, nausea, and numbness, so it is used as a last resort.
If the infection is bacterial, a course of oral antibiotics may be prescribed.
 Prevention
Prevention
To prevent the infection from recurring, you should:
- Wash your feet at least once a day, more frequently if they become sweaty, and
- Dry them thoroughly between the toes.
- Avoid tight footwear, especially in the summer. Sandals and “flip-flops” are the best warm weather footwear.
- Wear cotton or synthetic running socks which absorb sweat and change the socks daily or more frequently if they become damp.
- Dust an antifungal powder on your feet and into your shoes.
At home, it may help to wear open – toed shoes or go barefoot.
Related Links
Disclaimer
The Content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.