A felon is a severe infection of the pulpy tip of a finger, usually caused by infection with Staphylococcus 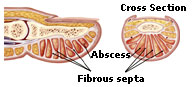 bacteria occurring as an abscess of the distal pulp. bacteria occurring as an abscess of the distal pulp.Fingertip pulp is divided into numerous small compartments by vertical septa that stabilize the pad. Infection occurring within these compartments can lead to abscess formation, edema, and rapid development of increased pressure in a closed space. This increased pressure may compromise blood flow and lead to necrosis of the skin and pulp. |
A felon usually is caused by inoculation of bacteria into the fingertip through a penetrating trauma. The most commonly affected digits are the thumb and index finger. Common predisposing causes include  Splinters,  Bits of glass, Bits of glass,Abrasions,  Minor puncture wounds. A puncture wound means you impaled yourself on some foreign body. Minor puncture wounds. A puncture wound means you impaled yourself on some foreign body. A felon also may arise when an untreated paronychia spreads into the pad of the fingertip. A felon also may arise when an untreated paronychia spreads into the pad of the fingertip. Felons have been reported following multiple finger-stick blood tests. Felons have been reported following multiple finger-stick blood tests. |
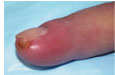 Patients present with rapid onset of severe, throbbing pain, with associated redness and swelling of the fingertip. The pain caused by a felon is usually more intense than that caused by paronychia. The swelling will not extend proximal to the distal interphalangeal joint. Occasionally, the high pressure in the fingertip pad will cause a felon to spontaneously drain, resulting in a visible sinus. Patients present with rapid onset of severe, throbbing pain, with associated redness and swelling of the fingertip. The pain caused by a felon is usually more intense than that caused by paronychia. The swelling will not extend proximal to the distal interphalangeal joint. Occasionally, the high pressure in the fingertip pad will cause a felon to spontaneously drain, resulting in a visible sinus.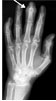 Bone and soft tissue radiographs should be obtained to evaluate for a foreign body If diagnosed in the early stages of cellulitis, Tetanus prophylaxis should be administered when necessary. 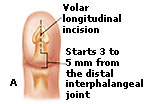 If fluctuance is present, incision and drainage are appropriate. The preferred techniques are a single volar longitudinal incision or a high lateral incision . Your doctor will make the whole finger numb by injecting an anesthetic once into each side of your finger, just beyond the knuckle of the hand. Then he or she will make one or more small cuts in the tip of your finger to allow the pus to drain out. A narrow gauze strip may be left in the wound to hold it open for continued drainage. The gauze may need to be replaced every day or two as it absorbs bacteria and debris from inside the wound. A doctor usually will prescribe antibiotics that work against “staph” bacteria infections, such as dicloxacillin (Dycill, Dynapen, Pathocil) or cephalexin (Biocef, Keflex, Keftab). If fluctuance is present, incision and drainage are appropriate. The preferred techniques are a single volar longitudinal incision or a high lateral incision . Your doctor will make the whole finger numb by injecting an anesthetic once into each side of your finger, just beyond the knuckle of the hand. Then he or she will make one or more small cuts in the tip of your finger to allow the pus to drain out. A narrow gauze strip may be left in the wound to hold it open for continued drainage. The gauze may need to be replaced every day or two as it absorbs bacteria and debris from inside the wound. A doctor usually will prescribe antibiotics that work against “staph” bacteria infections, such as dicloxacillin (Dycill, Dynapen, Pathocil) or cephalexin (Biocef, Keflex, Keftab).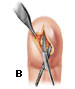 Incision techniques not recommended include the “fish-mouth” incision, the “hockey stick” (or “J”) incision, and the transverse palmar incision. These incisions are more likely to result in painful, sensitive scars and damage to neurovascular structures.  Postoperative care includes loose packing, splinting, and elevation of the hand for approximately 24 hours. Dry dressing changes with twice-daily saline soaks, range-of-motion activities and, eventually, scar massage may accelerate return to normal activity.The recommended length of treatment varies from five to 14 days and depends on the clinical response and severity of infection. Postoperative care includes loose packing, splinting, and elevation of the hand for approximately 24 hours. Dry dressing changes with twice-daily saline soaks, range-of-motion activities and, eventually, scar massage may accelerate return to normal activity.The recommended length of treatment varies from five to 14 days and depends on the clinical response and severity of infection.Consult a hand surgeon for more complex cases. |
Disclaimer
The Content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.



