“Mammography screening is not perfect but has been shown to markedly reduce the number of women each year who die from breast cancer,” said Elizabeth Morris, MD, FACR, president of the Society of Breast Imaging. “The decision whether or not to get a mammogram remains with women. We want them to know that mammography can detect cancer early — when it’s most treatable and can be treated less invasively — which not only saves lives but helps preserve quality of life.”
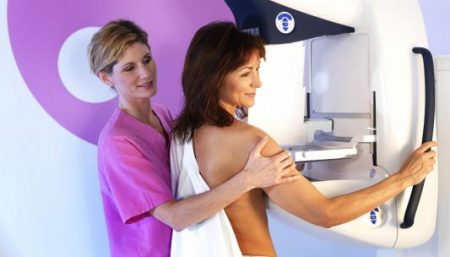
A mammogram is nothing else other than, an x-ray exam of the breast to detect and evaluate breast changes.
How is the Test Performed?
The test may find tumors that are too small to feel. During a mammogram, each breast is pressed between two plastic plates. Some discomfort is normal, but if it’s painful, tell the mammography technician. The best time to get a mammogram is at the end of your menstrual period. This is when your breasts are less tender. Some women have less breast tenderness if they don’t have any caffeine for a couple of days before the mammogram. After the x-ray pictures are taken, they are sent to a radiologist, who studies them and sends a report to your health care provider.
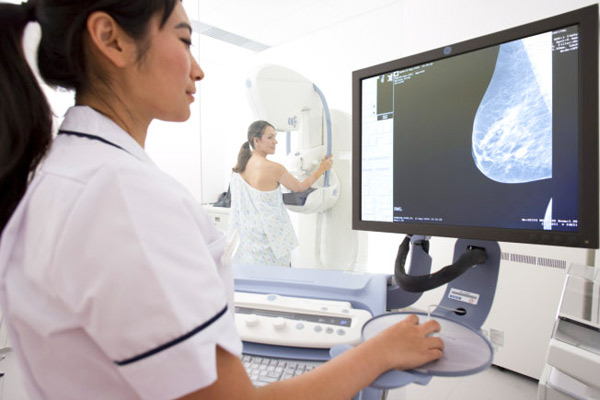
Both film and digital mammography use x-rays to make a picture of the breast tissue. The actual procedure for getting the mammogram is the same. The difference is in how the images are recorded and stored. It’s like the difference between a film camera and a digital camera. Film mammography stores the image directly on x-ray film. Digital mammography takes an electronic image of the breast and stores it directly in a computer. Digital images can be made lighter, darker, or larger. Images can also be stored and shared electronically.
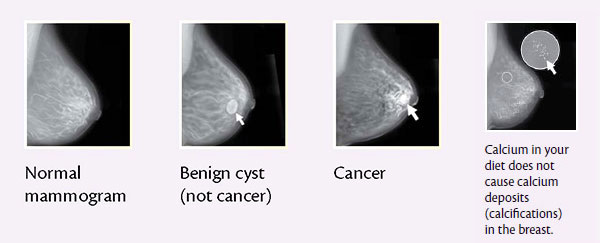
What can a mammogram show?
Mammograms can show lumps, calcifications, and other changes in your breast. The radiologist will study the mammogram for breast changes that do not look normal and for differences between your breasts. When possible, he or she will compare your most recent mammogram with past mammograms to check for changes. Mammography is a good tool to find breast changes in most women who have no signs of breast cancer. However, it does not detect all kinds of breast cancer, and many changes it finds are not cancer.
Risks
The main risk of mammograms is that they aren’t perfect. Normal breast tissue can hide a breast cancer so that it doesn’t show up on the mammogram. This is called a false negative. And mammography can identify an abnormality that looks like a cancer, but turns out to be normal. This “false alarm” is called a false positive. Besides worrying about being diagnosed with breast cancer, a false positive means more tests and follow-up visits, which can be stressful. To make up for these limitations, more than mammography is often needed. Women also need to practice breast self-examination, get regular breast examinations by an experienced health care professional, and, in some cases, also get another form of breast imaging, such as breast MRI or ultrasound.
To sum up in the simplest form, according to the WHO screening guidelines five key points should be applied to breast cancer and mammography:
- The disease being screened is serious and prevalent
- The test is sensitive and specific
- The test is well tolerated
- The test is inexpensive, and
- The test changes therapy or outcome.
Saving Women’s Lives.
http://www.cancer.gov/types/
Disclaimer
The Content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.