Blood clots (thrombus) play a dual role in an individuals life, one of a healthy lifesaver to stop excessive bleeding and that of death alarm if they migrate to your heart or lungs.
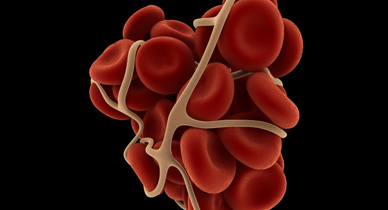
What Causes Blood Clots?
The process of blood clotting is triggered whenever flowing blood is exposed to certain substances. There are many different substances, which are called thrombogenic as they promote formation of thrombus (another name for a clot). These thrombogenic substances are located in the skin or in blood vessel walls. Normally safely separated from flowing blood, their contact with blood usually means the blood vessel wall is ruptured and bleeding. Examples of these thrombogenic substances are tissue factor, collagen, and von Willebrand factor.
Most heart attacks and strokes result from the sudden formation of a blood clot on a waxy cholesterol plaque inside an artery in the heart or brain. When the plaque ruptures suddenly, thrombogenic substances inside the plaque are exposed to blood, triggering the blood clotting process.
Blood clots may also form when blood fails to flow properly. Atrial fibrillation is an abnormal heart rhythm in which blood pools in the heart, potentially forming blood clots. If a blood clot dislodges and travels to the brain, it can cause a stroke. Prolonged immobilization can reduce blood flow in the legs, increasing the risk for blood clots in leg veins (deep venous thrombosis, or DVT). Deep Vein Thrombosis is a blood clot that forms in the deep veins of the legs most commonly, but can also occur in the veins of the upper extremities.
Risk Factors for a Blood Clot
- Long hours of immobility in case of air travel, long car rides and after surgery or a long illness. The longer those muscles go without contracting, the longer the blood stays there without being moved through the rest of your cardiovascular system.
- An injury that reduces blood flow to part of your body, such as a broken hip or leg
- Cancer, even during treatment
- Smoking
- A previous history of deep vein thrombosis or pulmonary embolism
- An inherited condition that increases blood clotting
- Paralysis from a spinal cord injury
- Current use of hormone therapy, including that used for postmenopausal symptoms, especially in smokers
- Pregnancy or having recently given birth, especially by C-section
- Varicose veins, which are swollen, twisted, painful veins
- A history of heart attack, stroke, or congestive heart failure
- Inflammatory bowel disease
- Extra weight
- Current use of birth control pills or patches
Preventive Tips
 1. Avoid Sitting for Longer Durations: If you have been sitting for a while in a particular posture, involve mobility because this can limit blood flow. If you’re traveling a long distance by car, stop every hour or so and walk around. If you’re on a plane, try to stand or walk occasionally. If you can’t do that, at least try to exercise your lower legs. Try raising and lowering your heels while keeping your toes on the floor, then raising your toes while your heels are on the floor.
1. Avoid Sitting for Longer Durations: If you have been sitting for a while in a particular posture, involve mobility because this can limit blood flow. If you’re traveling a long distance by car, stop every hour or so and walk around. If you’re on a plane, try to stand or walk occasionally. If you can’t do that, at least try to exercise your lower legs. Try raising and lowering your heels while keeping your toes on the floor, then raising your toes while your heels are on the floor.
2. Maintain an active lifestyle and exercise regularly — daily, if possible. If you are sedentary, it will affect your blood flow and increase your risk for deep vein thrombosis. The risk is added on if you are obese and pregnant. Walking, swimming, and bicycling are all great activities.
3. Manage your weight with exercise as well as by eating a healthy diet. Obese people are at an increased risk of blood clots and diseases such as stroke. In the study, conducted by Colorado investigators three months of walking about 45 minutes a day, five days a week — 10 of the obese men had a 50% higher release of blood clot-dissolving t-PA. In fact, exercise raised their levels similar to those of the lean men.
4. If you smoke, quit! Dr Yun-Jiu Cheng, MD, from the Department of Cardiology at Sun Yat-sen University in China reported in his study “smoking increased the risk of developing a deep vein blood clot, and that the more cigarettes a person smoked, the greater the risk for developing the clot.”Nicotine therapy (in patches, gums, or sprays) and support groups can make this much easier to do.
5. Get your blood pressure checked regularly; take steps to lower it, if necessary.
6. Report any family or personal history of blood-clotting problems to your doctor.
 7. Discuss alternatives to birth control pills or hormone-replacement therapy with your doctor. Have an honest chat about your medical history and concerns with your provider to make an informed and safe decision about using birth control and what method is best for you. During your next annual exam talk about contraceptive options. You can also decide to make an appointment specifically to discuss birth control, clots and your personal risk.
7. Discuss alternatives to birth control pills or hormone-replacement therapy with your doctor. Have an honest chat about your medical history and concerns with your provider to make an informed and safe decision about using birth control and what method is best for you. During your next annual exam talk about contraceptive options. You can also decide to make an appointment specifically to discuss birth control, clots and your personal risk.
8. Take anticoagulants to prevent a blood clot if you are recovering after some types of surgery.
9. Use compression stockings to help prevent DVT if you are at an increased risk.
10. Stay Hydrated. Drink plenty of fluids and avoid alcohol. Dehydration causes blood vessels to narrow and blood to thicken, raising risk for blood clots.
|
Sitting Leg Exercises When you can’t walk, here are movements you can do while seated. Foot pumps. Place your feet flat on the floor, and then raise your toes toward you and hold for a few seconds. Lower your toes and balls of your feet to the floor, then raise your heels and hold for another few seconds. Ankle circles. Raise both feet off the floor and trace a circle with your toes. You could also trace each letter of the alphabet to keep yourself occupied, Robertson said. Leg raises. If you have room in front of you, raise your left foot off the floor. Straighten the leg slowly, then return your foot back on the floor. Repeat with your right leg. Alternatively, slowly lift your left knee up to your chest, then bring your foot back to the floor; repeat with your right leg. Shoulder rolls. Although you’re less likely to form a clot in your upper body, it doesn’t hurt to keep your blood flowing there. Simply raise your shoulders and circle them back and down five times. Then reverse direction for five more repetitions. |
Ref:
Related Links
- Deep-Vein Thrombosis
- Top 10 anywhere leg exercises
- Yaz and Yasmin: Two Controversial Birth Control Pills
- Get ready to spice up your walking program
Disclaimer
The Content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.