What is Trigeminal Neuralgia ?
Severe pain on one side of the face due to compression, inflammation, or damage to the trigeminal nerve.
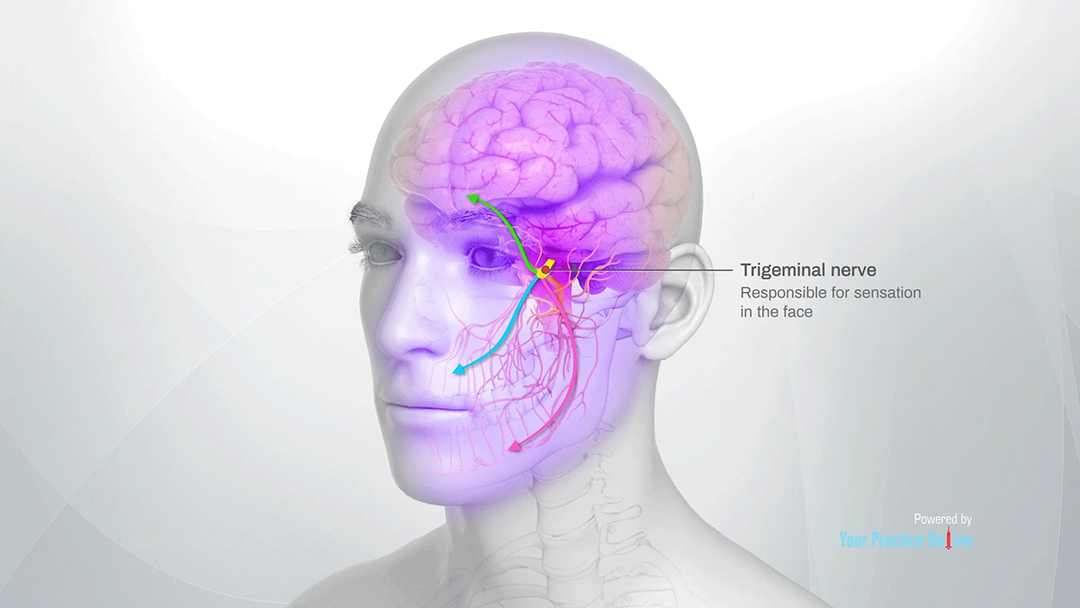
The trigeminal nerve transmits sensation from parts of the face to the brain and controls some of the muscles that are involved in chewing.
TN (Trigeminal Neuralgia / tic douloureux) is a disorder of the fifth cranial (trigeminal) nerve that causes episodes of intense, stabbing, electric shock-like pain in the areas of the face where the branches of the nerve are distributed – lips, eyes, nose, scalp, forehead, upper jaw, and lower jaw. By many, it’s called the “suicide disease”.
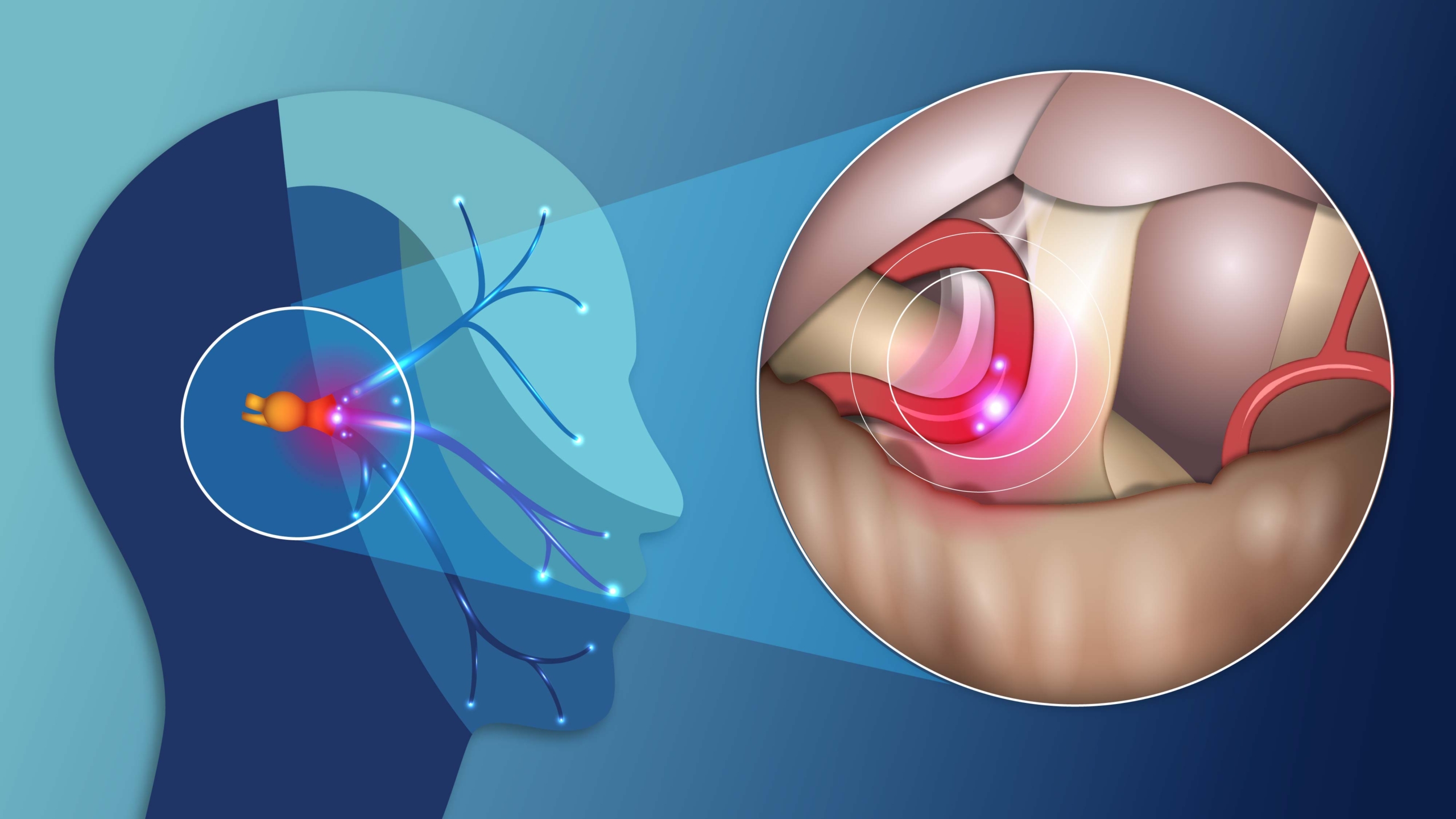
Where lies the Trigeminal Nerve?
The trigeminal nerve is the fifth of twelve pairs of cranial nerves enervating the face and head, and is denoted by the Roman Numeral V. It has three divisions which enervate the forehead and eye (ophthalmic V1), cheek (maxillary V2) and lower face and jaw (mandibular V3). The trigeminal nerves function in sensing facial touch, pain and temperature, as well as controlling muscles used for chewing. The trigeminal nerve functions should be distinguished from the facial nerve (cranial nerve VII), which controls all other facial movements.
The three divisions of the trigeminal nerve come together in an area called the Gasserion ganglion. From there, the trigeminal nerve root continues back towards the side of the brain stem, and inserts into the pons. Within the brain stem, the signals traveling through the trigeminal nerve reach specialized clusters of neurons called the trigeminal nerve nucleus. Information brought to the brain stem by the trigeminal nerve is then processed before being sent up to the brain and cerebral cortex, where a conscious perception of facial sensation is generated.
Types of Trigeminal neuralgia
There are seven forms of TN:
These forms of TN can be distinguished from idiopathic (atypical) facial pain, as well as other disorders causing cranio-facial pain.
1- Typical TN- This is the most common form of TN, that has previously been termed Classical, Idiopathic and Essential TN. Nearly all cases of typical TN are caused by blood vessels compressing the trigeminal nerve root as it enters the brain stem.
2- Atypical TN- Atypical TN is characterized by a unilateral, prominent constant and severe aching, boring or burning pain superimposed upon otherwise typical TN symptoms. Some believe atypical TN is due to vascular compression upon a specific part of the trigeminal nerve (the portio minor), while others theorize that atypical TN represents a more severe form or progression of typical TN.
3- Pre-TN- Days to years before the first attack of TN pain, some sufferers experience odd sensations in the trigeminal distributions destined to become affected by TN. These odd sensations of pain, (such as a toothache) or discomfort (like “pins and needles”, parasthesia), may be symptoms of pre-trigeminal neuralgia. Pre-TN is most effectively treated with medical therapy used for typical TN. When the first attack of true TN occurs, it is very distinct from pre-TN symptoms.
4- Multiple-sclerosis-related TN– Two to four percent of patients with TN have evidence of multiple sclerosis and about 1% of patients suffering from multiple sclerosis develop TN. Those with MS-related TN tend to be younger when they experience their first attack of pain, and the pain progresses over a shorter amount of time than in those with typical TN. Furthermore, bilateral TN is more commonly seen in people with multiple sclerosis.
5- Secondary TN or Tumor Related Trigeminal Neuralgia- Trigeminal neuralgia pain caused by a lesion, such as a tumor, is referred to as secondary trigeminal neuralgia. A tumor that severely compresses or distorts the trigeminal nerve may cause facial numbness, weakness of chewing muscles, and/or constant aching pain (also see Trigeminal Neuropathy or Post-Traumatic Trigeminal Neuralgia).
6- Trigeminal Neuropathy or Post-traumatic TN (trigeminal neuropathy)- Trigeminal Neuropathy or Post-Traumatic TN may develop following cranio-facial trauma (such as from a car accident), dental trauma, sinus trauma (such as following Caldwell Luc procedures) but most commonly following destructive procedures (rhizotomies) used for treatment of TN. Following TN injury, numbness may become associated with bothersome sensations or pain, sometimes called phantom pain or deafferentation pain. These pain conditions are caused by irreparable damage to the trigeminal nerve and secondary hyperactivity of the trigeminal nerve nucleus
7- Failed TN- Unfortunately, in a very small proportion of sufferers, all medications, microvascular decompression and destructive rhizotomy procedures prove ineffective in controlling TN pain. This condition is called “failed” trigeminal neuralgia. Such individuals also often suffer from additional trigeminal neuropathy or post-traumatic TN as a result of the destructive interventions they underwent.
Causes of Trigeminal neuralgia
The pain of trigeminal neuralgia is due to a disturbance in the function of the trigeminal nerve, which carries sensation from the face to the brain. The cause of the pain is often unknown. But, the pain may occur when a blood vessel comes in contact with the trigeminal nerve. This places pressure on the main part of the nerve as it enters the brain.
Besides pressure by a blood vessel, other less frequent sources of pain to the trigeminal nerve may include:
Compression by a tumor.
Inflammation, swelling and injury of the covering (myelin sheath) of the trigeminal nerve in a process called demyelination. This occurs in people with multiple sclerosis who develop trigeminal neuralgia.
Symptoms of Trigeminal neuralgia
Damage to this nerve causes repeated bursts of sharp, stabbing pain, known as trigeminal neuralgia, in the lip, gum, or cheek on one side of the face. Attacks may last for a few seconds or several minutes and may become more frequent over time. An attack may occur spontaneously or be triggered by certain facial movements, such as chewing, or by touching a trigger spot on the face. Attacks rarely occur at night.
People who have experienced severe trigeminal neuralgia have described the pain as:
- Lightning-like
- Shooting
- Jabbing
- Like having live wires in your face
It’s possible for the pain to occur on both sides of your face, but trigeminal neuralgia usually affects just one side. The pain may affect just a portion of one side of your face, or the pain may spread in a wider pattern.
The condition also tends to come and go. You may experience attacks of pain off and on all day, or even for days or weeks at a time. Then, you may experience no pain for a prolonged period of time.
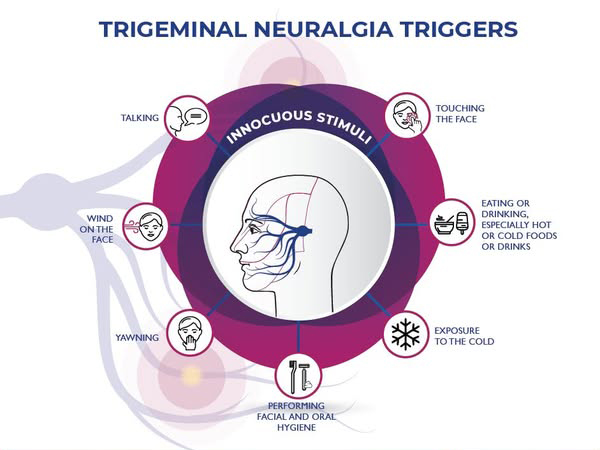
A variety of triggers, many subtle, may set off the pain. These triggers may include:
- Shaving
- Stroking your face
- Eating
- Drinking a hot or cold liquid
- Brushing your teeth
- Talking
- Putting on makeup
- Encountering a slight breeze
- Walking into an air-conditioned room
Diagnosis of Trigeminal neuralgia
No one test can diagnose trigeminal neuralgia. The condition must be distinguished from other forms of facial pain that may be due to diseases of the teeth, jaw or sinuses. Magnetic resonance imaging (MRI) or computerized tomography (CT) scans of the brain can eliminate some causes, such as tumors, aneurysms or multiple sclerosis, all of which can cause trigeminal neuralgia in a small number of people.
Your doctor will examine you to rule out any other causes of facial pain, such as toothache or sinusitis .
A physician will ask for a description of the pain — how severe it is, what part of the face it affects, what seems to trigger episodes of pain. A neurologic examination involves touching various parts of the face to determine exactly where the pain is occurring and — if it appears to be trigeminal neuralgia — which branches of the trigeminal nerve may be affected.
Treatment of Trigeminal neuralgia
Medications are the typical initial treatment for trigeminal neuralgia. Medications are often effective in lessening or blocking the pain signals sent to your brain. A number of drugs are available. If you stop responding to a particular medication or experience too many side effects, there’s always the potential to switch to another one.
Your doctor may prescribe painkillers, such as paracetamol or ibuprofen.
However, if the pain persists, your doctor may prescribe anticonvulsant drugs, such as carbamazapine, Phenytoin (Dilantin, Phenytex, Oxcarbazepine (Trileptal) or certain antidepressants, all of which have been shown to be effective in treating trigeminal neuralgia. Unlike painkillers, which are taken only when the pain is present, both anticonvulsants and antidepressants need to be taken every day to prevent attacks.
Baclofen (Lioresal) a muscle relaxant may be used in combination with carbamazepine or phenytoin. Side effects include confusion, mental depression and severe drowsiness.
If a tumour is found, surgery may be necessary to remove it. Surgery may also be used to separate the trigeminal nerve from a blood vessel if the vessel is compressing the nerve. The goal of a number of surgical procedures is to either damage or destroy the part of the trigeminal nerve that’s the source of the pain. Because the success of these procedures depends on damaging the nerve, one side effect is facial numbness of varying degrees.
These procedures involve:
Alcohol injection. Alcohol injections under the skin of your face at the areas of pain may offer temporary pain relief by numbing the areas for days or months. Because the pain relief isn’t permanent, you may need repeated injections.
Glycerol injection. This procedure is called percutaneous glycerol rhizotomy (PGR), Percutaneous means through the skin. Your doctor inserts a needle into the trigeminal cistern (a small sac of spinal fluid that contains the trigeminal nerve ganglion and part of its root). Images are made to confirm that the needle is in the proper location. Once the location is confirmed, your doctor injects a small amount of sterile glycerol. After 3 or 4 hours, the glycerol damages the trigeminal nerve and blocks pain signals.
Initially, PGR relieves pain. However, many people have a recurrence of pain, and many experience mild facial numbness or tingling.
Balloon compression. In a procedure called percutaneous balloon compression of the trigeminal nerve (PBCTN), your doctor inserts a hollow needle through your face and into an opening in your skull. Then a thin, flexible tube (catheter) with a balloon on the end is threaded through the needle. The balloon is inflated with enough pressure to damage the nerve and block pain signals.
PBCTN successfully controls pain in most people. Only a small number of people experience a recurrence of pain. Most people undergoing PBCTN experience facial numbness of varying degrees, and more than half experience nerve damage, resulting in a temporary weakness in the muscles used to chew.
Electric current. A procedure called percutaneous stereotactic radiofrequency thermal rhizotomy (PSR) selectively destroys nerve fibers associated with pain. Your doctor threads a needle through your face and into an opening in your skull. Once in place, an electrode is threaded through the needle until it rests against the nerve root.
The electrode is positioned so that you experience numbness or pain. An electric current is passed through the tip of the electrode until it is heated to the desired temperature for about 70 seconds. This damages the nerve fibers and creates an area of injury (lesion). If your pain isn’t eliminated, your doctor may create additional lesions.
PSR successfully controls pain in most people. A common side effect of this type of treatment is mild to severe facial numbness.
Radiation. Gamma knife radiosurgery (GKR) involves delivering single high doses of radiation to the root of the trigeminal nerve. The radiation damages the trigeminal nerve and eliminates the pain. GKR is successful in eliminating pain more than half of the time. The procedure is painless and typically is done without anesthesia. Because it’s relatively new, the long-term risks of this type of radiation are not yet known.
Severing the nerve. Your doctor may work through a small incision to cut the branch of the trigeminal nerve that’s causing the pain as that nerve branch leaves your skull and before it reaches your facial area. Attacks neuralgia may stop spontaneously, become more frequent, or persist unchanged for months or years. However, symptoms usually improve significantly with treatment.

Microvascular decompression (MVD)
A procedure called microvascular decompression (MVD) doesn’t damage or destroy part of the trigeminal nerve. Instead, MVD involves relocating or removing blood vessels that have contact with the trigeminal root and separating the root and vessels with a small pad.
During MVD, your doctor makes a small incision behind one ear. Then, through a quarter-sized hole in your skull, part of your brain is lifted to expose the trigeminal nerve. If your doctor finds an artery in contact with the nerve root, he or she directs it away from the nerve and places a pad between the nerve and the artery. Doctors usually remove an artery that is found to be compressing the trigeminal nerve.
MVD can successfully eliminate or reduce pain almost all of the time, but as with every other surgical procedure for trigeminal neuralgia, pain can recur in some people.
While MVD has a high success rate, it also carries risks. There are small chances of decreased hearing, facial weakness, facial numbness, double vision and even a stroke or death.
Disclaimer
The Content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.