
Gestational diabetes is a carbohydrate intolerance of variable severity that starts or is first recognized during pregnancy or the inability of the tissues to absorb glucose from the bloodstream during pregnancy due to a lack of the hormone insulin.
The new guidelines are based on a study of more than 23,000 women in nine countries. Metzger and the international team concluded that:
- A fasting blood sugar level of 92 or higher,
- A one-hour level of 180 or higher on a glucose tolerance test, or
- A two-hour level of 153 or higher on a glucose tolerance test
All posed serious risks to the mother and the infant. All of these levels had previously been considered to be in the safe, normal range, and a woman had to have two high levels before she would be diagnosed with gestational diabetes.
(The study’s lead author Boyd Metzger, MD, the Tom D. Spies Professor of Metabolism and Nutrition at Feinberg and a physician at Northwestern Memorial Hospital, and a group of 50 international experts spent about two years analyzing data from a 2008 study. )
Causes:

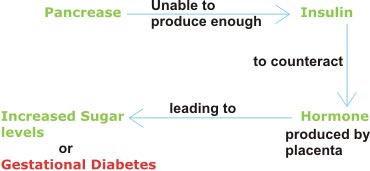
Glucose is a form of sugar that is present in many foods, including sweets, potatoes, pasta, and breads. The body uses glucose to provide energy. It is stored in the liver, muscles, and fatty tissue. The pancreas produces a hormone (a chemical produced in one part of the body, which travels to another part of the body in order to exert its effect) called insulin. Insulin is required to allow glucose to enter the liver, muscles, and fatty tissues, thus reducing the amount of glucose in the blood. In diabetes, blood levels of glucose remain abnormally high. In many forms of diabetes, this is because the pancreas does not produce enough insulin.
In gestational diabetes, the pancreas is not at fault. Instead, the problem is in the placenta. During pregnancy, the placenta provides the baby with nourishment. It also produces a number of hormones that interfere with the body’s usual response to insulin. This condition is referred to as “insulin resistance.” Most pregnant women do not suffer from gestational diabetes, because the pancreas works to produce extra quantities of insulin in order to compensate for insulin resistance. However, when a woman’s pancreas cannot produce enough extra insulin, blood levels of glucose stay abnormally high, and the woman is considered to have gestational diabetes.
Women at risk:

During the course of pregnancy, up to 1 in 50 women temporarily develop diabetes mellitus.
Women at risk for gestational diabetes include those who:
- are overweight
- have a family history of diabetes
- have previously given birth to a very large, heavy baby
- have previously had a baby who was stillborn, or born with a birth defect
- have an excess amount of amniotic fluid (the cushioning fluid within the uterus that surrounds the developing fetus)
- are over 25 years of age
- belong to an ethnic group known to experience higher rates of gestational diabetes (in the United States, these groups include Mexican-Americans, American Indians, African-Americans, as well as individuals from Asia, India, or the Pacific Islands)
- have a previous history of gestational diabetes during a pregnancy.
| The IADPSG guidelines recommend screening all women at their first doctor’s visit early in pregnancy, using the current criteria to diagnose diabetes in the general population. The goal here is to identify diabetes that is already present but not diagnosed. These women are already diabetic, and care should be started to control their blood sugar. The guidelines then suggest doing a full glucose tolerance test in the second trimester of pregnancy, without doing the screen with the small amount of glucose first. |
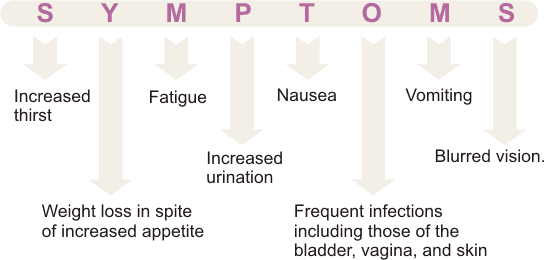
Symptoms:

Most women with gestational diabetes have no recognizable symptoms for this reason it is recommended that all pregnant women be screened for gestational diabetes during the 24th and 28th weeks of their pregnancy.
The symptoms are usually mild and not life-threatening to the pregnant woman like
Diagnosis:

The current guidelines of the American Diabetes Association (ADA) recommend screening women in the second trimester of pregnancy (after about 20-24 weeks of pregnancy). By this point in the pregnancy, the placental hormones have reached a sufficient level to cause insulin resistance. It involves the pregnant woman drinking a special solution that contains exactly 50 grams of glucose. An hour later, the woman’s blood is drawn and tested for its glucose level. A level less than 140 mg/dl is considered normal.
When the screening glucose level is over 140 mg/dl, a special three-hour glucose tolerance test is performed. This involves following a special diet for three days prior to the test. This diet is set-up to contain at least 150 grams of carbohydrate each day. Just before the test, the patient is instructed to eat and drink nothing (except water) for 10-14 hours. A blood sample is then tested to determine the fasting glucose level. The patient then drinks a special solution containing exactly 100 grams of glucose, and her blood is tested every hour for the next three hours. If two or more of these levels are elevated over normal, then the patient is considered to have gestational diabetes.
A recent article from an international panel of experts, known as the International Association of Diabetes and Pregnancy Study Group (IADPSG), has suggested new guidelines for diagnosing gestational diabetes. According to them a woman may not need laboratory testing to screen for GDM if she meets all of the following criteria:
- less than 25 years old
- not a member of a racial or ethnic group with a high prevalence of diabetes (eg, Hispanic, African, Native American, South or East Asian, or Pacific Islands ancestry)
- a body mass index (BMI) 25
- no history of abnormal glucose tolerance
- no previous history of adverse pregnancy outcomes usually associated with GDM
- no known diabetes in first-degree relative
Women who are at a higher risk for GDM usually have one of the following risk factors:
- age
- ethnicity
- obesity
Treatment:
Treatment for gestational diabetes will depend on the severity of the diabetes. The goals of treatment are to maintain blood glucose levels within normal limits during the duration of the pregnancy, and ensure the well-being of the fetus.


Diet:
Mild forms can be treated with diet (decreasing the intake of sugars and fats, in particular). The overall principles are to reduce the amount of fat, simple sugar, and salt and increase the amount of complex carbohydrates and foods high in fiber. Current American Diabetes Association guidelines advise that less than 30% of total daily calories should come from fat sources. Protein choices with less fat are recommended, such as skinless poultry, fish, and lean meats. The recommended daily allowance is approximately two three-ounce servings of protein a day. A three-ounce portion of meat is approximately the size of a deck of playing cards. No more than 10% to 20% of the day’s total calories should come from protein. Approximately 50% to 60% of the day’s total calories should come from complex carbohydrates such as starches and whole-grain breads, with an emphasis on the high-fiber choices. Foods that are high in carbohydrates provide energy, minerals, and vitamins. Food sources of complex carbohydrates and fiber are fruits and vegetables, whole-grain breads and cereals, dried beans and peas, and lentils and legumes. Meals should be eaten at approximately the same time every day.
Use sources of simple (concentrated) carbohydrates, such as table sugar, honey, soda, juice, or syrup, in moderation. Concentrated sources of carbohydrates cause the blood sugar levels to rise quickly. Exercise caution when eating simple carbohydrates. A registered dietitian can help you best decide how to include simple carbohydrates into your diet plan.
ACOG state quite clearly that even if one chooses to restrict caloric intake no more than 33% of the calories should be removed from the woman’s diet.
Here are some other guidelines:
- Eat and drink at least 4 servings of dairy products and calcium-rich foods a day to help ensure that you are getting 1200 mg. of calcium in your daily diet.
- Drink at least 8 cups (or 64 ounces) of liquids per day.
- Eat at least three servings of iron-rich foods per day to ensure you are getting 30 mg. of iron in your daily diet.
- Choose at least one source of Vitamin C every day.
- Choose at least one source of folic acid every day.
- Choose at least one source of Vitamin A every other day.
- Eat three small meals and two or three snacks at regular times every day. Do not skip meals or snacks.
- Avoid alcoholic beverages during pregnancy. Alcohol has been linked to premature delivery and low birth weight babies.
- Limit caffeine to no more than 300 mg. per day
- DO NOT DIET or try to lose weight during pregnancy.
- Eat a variety of foods to get all the nutrients you need.
Exercise:

Regular physical activity is sometimes used to keep blood sugar levels lower because contracting muscles help stimulate glucose transport. In the absence of either medical or obstetrical contraindications, exercise prescription can be an alternative or adjunct therapy for women who have gestational diabetes. Non-weight-bearing exercises such as stationary cycling, swimming, and arm exercises, may be most suitable for these patients, to improve and maintain glucose homeostasis. Walking may be another safe option. For more, click here
Try exercising frequently, 4 to 5 days per week, to get the “blood sugar lowering” advantages of an exercise program. Don’t omit a warm-up period of 5 to 10 minutes and a cool-down period of 5 to 10 minutes. Always stop exercising if you feel pain, dizziness, shortness of breath, faintness, palpitations, back or pelvic pain, or experience vaginal bleeding. Also, avoid vigorous exercise in hot, humid weather or if you have a fever. It is important to prevent dehydration during exercise, especially during pregnancy. The American College of Obstetricians and Gynecologists (ACOG) recommends drinking fluids prior to and after exercise, and if necessary, during the activity to prevent dehydration. The maternal heart rate not exceed 140 beats per minute. Along with the exercise program, women with gestational diabetes should follow a daily balanced American Diabetes Association diet of 30 kcal/kg ideal body weight.
Because both insulin and exercise lower blood sugar levels, the combination can result in hypoglycemia or low blood sugar. Therefore, when exercising, take along sugar in the form of hard, sugar-sweetened candies just in case your blood sugar becomes too low. If on insulin, you should always carry some form of sugar for potential episodes of hypoglycemia.
Medication:

When diet and exercise do not keep blood glucose levels within an acceptable range, a patient may need to take regular shots of insulin. Self-monitoring of blood glucose is required for effective treatment with insulin. Patients are often asked to regularly measure their blood sugar. This is done by poking a finger with a needle called a lancet, putting a drop of blood on a special type of paper, and feeding the paper into a meter which analyzes and reports the blood sugar level. A good glucose meter company will inform you about the different meter choices if you do not want to poke your finger everyday.”
Prevention:
There is no known way to actually prevent diabetes, particularly since gestational diabetes is due to the effects of normal hormones of pregnancy. However, the effects of insulin resistance can be best handled through careful attention to diet, avoiding becoming overweight throughout life, and participating in reasonable exercise.
Source:
- Mayo Clinic
- National Institute of Diabetes, and Digestive and Kidney Diseases
- Northwestern University Feinberg School of Medicine
- International Association of Diabetes and Pregnancy Study Groups Recommendations on the Diagnosis and Classification of Hyperglycemia in Pregnancy. Diabetes Care. March 3, 2010. Pages 675-682.
Disclaimer
The Content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition.



