What causes Alzheimer’s disease? The answer could be right under our noses, says leading expert Professor Ruth Itzhaki. Her latest paper presents a lifetime of research evidence that the herpes virus responsible for cold sores can also cause Alzheimer’s — and new data which show antiviral drugs drastically reduce risk of senile dementia in patients with severe herpes infections.
The review in Frontiers in Ageing Neuroscience raises the tantalizing prospect of a simple, effective preventive treatment for one of humanity’s costliest disorders. The HSV1 theory of Alzheimer’s disease Herpes viruses are the dreaded ‘gift that keeps on giving’. They remain lifelong in our neurons and immune cells, reactivating and resurfacing in characteristic blisters when we’re run down by stress or illness. Most people are infected by Herpes Simplex Virus 1 (HSV1) by the time they reach old age.
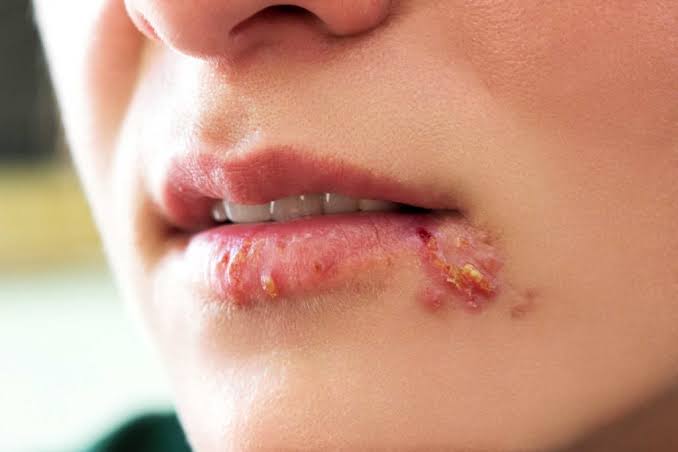
But what happens to infected neurons in our brain during this reactivation? “HSV1 could account for 50% or more of Alzheimer’s disease cases,” says Professor Itzhaki, who has spent over 25 years at the University of Manchester investigating a potential link. HSV1 is better known as the cause of cold sores. Itzhaki has shown previously that cold sores occur more frequently in carriers of APOE-ε4 — a gene variant that confers increased risk of Alzheimer’s. “Our theory is that in APOE-ε4 carriers, reactivation is more frequent or more harmful in HSV1-infected brain cells, which as a result accumulate damage that culminates in development of Alzheimer’s.”
Proving the theory Few countries collect the population data required to test this theory — for example, to find out whether antiviral treatments reduce dementia risk. In Taiwan however, researchers have done just that. There, 99.9% of the population is enrolled in a National Health Insurance Research Database, which is being extensively mined for information on microbial infections and disease. In 2017-2018 three studies were published describing Taiwanese data on the development of senile dementia — of which Alzheimer’s is the main cause — and the treatment of patients with marked overt signs of infection with HSV or varicella zoster virus (VZV, the chickenpox virus). “The striking results include evidence that the risk of senile dementia is much greater in those who are infected with HSV, and that anti-herpes antiviral treatment causes a dramatic decrease in number of those subjects severely affected by HSV1 who later develop dementia.”
Previous findings from Itzhaki’s own research group provide a mechanistic link which supports these epidemiological findings. They found that HSV1 causes protein deposits characteristic of Alzheimer’s: ‘plaques’ between neurons, and ‘tangles’ inside of them. “Viral DNA is located very specifically within plaques in postmortem brain tissue from Alzheimer’s sufferers. The main proteins of both plaques and tangles accumulate also in HSV1-infected cell cultures — and antiviral drugs can prevent this.” Towards a cure “It should be stressed that the results of these Taiwanese studies apply only to severe HSV1 (or VZV) infections, which are rare,” admits Itzhaki. “Ideally, we would study dementia rates amongst people who have suffered mild HSV1 infection, including herpes labialis (cold sores) or mild genital herpes, but these are far less likely to be documented.” Although further work is needed to confirm and define a causal link between HSV1 infection and Alzheimer’s, Itzhaki is enthusiastic about the treatment prospects. “Considering that over 150 publications strongly support an HSV1 role in Alzheimer’s, these Taiwan findings greatly justify usage of antiherpes antivirals — which are safe and well-tolerated — to treat Alzheimer’s disease. “They also incentivize development of an HSV1 vaccine, which would likely be the most effective treatment.” This echoes the growing use worldwide of human papillomavirus (HPV) vaccination to prevent cervical cancer — another virus-disease link which emerged in a similar process of research.